Back Pain: Intervertebral Disc Disease and
the
Cavalier King Charles Spaniel
-
 What It Is
What It Is - Symptoms
- Diagnosis
- Grading IVDD
- DNA Testing
- Related Disorders
- Treatment
- Research News
- Related Links
- Veterinary Resources
Intervertebral disc disease* (IVDD) is progressive degeneration of the discs (or disks) between the vertebrae (spondyle) of the spine. Cavalier King Charles spaniels are reportedly prone to a form of IVDD known as Hansen Type I intervertebral disc disease. IVDD is most common in the Dachshund, beagle and French bulldog. IVDD tends to affect cavaliers suddenly and in their later years -- after age 5 years -- and in the region of their neck.
A similar condition is an extruded disc due to other causes, such as injuries. This is called intervertebral disc extrusion (IVDE). In most cases, IVDE may more often affect younger cavaliers. See this February 2024 article.
Other consequences of this degeneration are chronic disorders called spondylosis and spondyloarthropathy. IVDD) is the most frequent cause of acute paralysis in dogs, accounting for 70% of cases on a species-wide basis. See this May 2020 article.
To a more limited extent, young cavaliers also have been diagnosed with a congential disorder of the vertebrae known as dsyplastic caudal vertebral articular process, a compression of the spinal cord within the thoracic vertebrae. See this May 2005 article and this October 2019 article.
* IVDD also is referred to as degenerative disc disease (DDD) and intervertebral disc herniation (IVDH).
What It Is
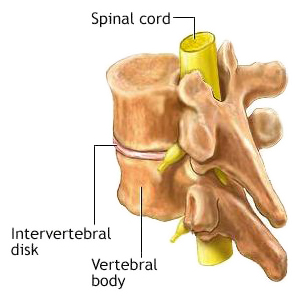
The intervertebral
disc is a puck-shaped, shock absorbing and
stabilizing cushion between most of the vertebrae (the bones of the spine). Each
disc consists of a tough outer layer (fibrous tissues and cartilage,
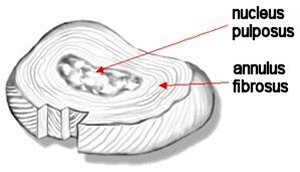 called
anulus fibrosus) which
surrounds a spongy inner core (gelatinus and cartilage, called nucleus pulposus).
called
anulus fibrosus) which
surrounds a spongy inner core (gelatinus and cartilage, called nucleus pulposus).
For the typical dog, its discs may survive intact or may deteriorate very gradually over its lifetime. However, for some breeds, including the cavalier King Charles spaniel, one or more of the dog’s discs’ outer layer may start to degenerate at a younger age and progress more rapidly, causing the inner core to narrow and harden. As the degeneration of the disc progresses, the outer layer may rupture, allowing the hardened inner core to extrude (herniate) and compress the adjacent spinal cord and nerve roots, causing pressure, inflammation, and pain.
![]() For a thorough review of all classes of intervertebral disc diseases, see
this October 2020
article. See, also, this
YouTube video by Dr. Clare Rusbridge.
For a thorough review of all classes of intervertebral disc diseases, see
this October 2020
article. See, also, this
YouTube video by Dr. Clare Rusbridge.
Hansen Type I (IVDE)
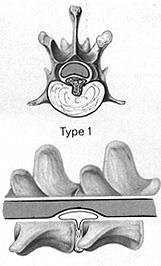 This early progression of the degenerating disc is called
Hansen Type I intervertebral disc disease (IVDD)
* (see at right). This disorder
occurs primarily in chondrodystrophic breeds (which include the Cocker spaniel, Basset hound,
beagle, bulldogs, Corgi, Dachshund, Shih-Tzu and Pekingese).
This early progression of the degenerating disc is called
Hansen Type I intervertebral disc disease (IVDD)
* (see at right). This disorder
occurs primarily in chondrodystrophic breeds (which include the Cocker spaniel, Basset hound,
beagle, bulldogs, Corgi, Dachshund, Shih-Tzu and Pekingese).
* Hansen Type I intervertebral disc disease may also be referred to as "Hansen type I intervertebral disc extrusion (IVDE)" in some veterinary publications. See this July 2022 ACVIM Consensus Statement.
RETURN TO TOP
Chondrodystrophy (CDDY)
Chondrodystrophy (CDDY) is a disorder of the formation of cartilage, which is the connective tissue between bones. The cartilage development of chondodystrophic breeds is genetically deformed, as a consequence of having been bred for shorter legs and other characteristics of dwarfism. A mutation of the gene called Fibroblast growth factor 4 (FGF4), is considered to be responsible for chondrodystrophy. See the DNA Testing section below of details.
In reports on the subject of chondrodystrophic breeds, cavalier King Charles spaniels have been described as being either chondrodystropic-type or semi-chondrodystrophic. Regardless of where CKCSs fit within the spectrum of chondrodystrophic breeds, they suffer from Hansen Type I IVDD nearly as often as some breeds clearly identifiable as being chondrodystrophic.
In chondrodystrophic breeds, degeneration of the disc occurs as a result of this cartilage deformity, and it usually occurs at relatively young ages, such as between ages 3 and 6 years, and it tends to recur periodically, in multiple areas along the spine. It usually comes on suddenly and is very painful.
RETURN TO TOP
Lumbosacral Stenosis
The lumbosacral joint of the spinal column is the junction between
the last lumbar vertebra – L7 – and the sacrum, a triangular shaped bone
that consists of 5 vetebrae and a section of the pelvis. A high amount
of stress
 is
imposed upon this joint and its lumbosacral intervertebral disc, which
can lead to degeneration of that disc as the dog ages, resulting in
protrusion of the disc and compression of the spinal cord at that point.
This condition is labeled “canine degenerative lumbosacral stenosis”
(DLSS). In most cases, it is categorized as a form of Hansen Type II
IVDD, but cavaliers have been described as developing DLSS as a case of
Hansen Type I.
is
imposed upon this joint and its lumbosacral intervertebral disc, which
can lead to degeneration of that disc as the dog ages, resulting in
protrusion of the disc and compression of the spinal cord at that point.
This condition is labeled “canine degenerative lumbosacral stenosis”
(DLSS). In most cases, it is categorized as a form of Hansen Type II
IVDD, but cavaliers have been described as developing DLSS as a case of
Hansen Type I.
In this March 2021 article, a cavalier was among 13 dogs diagnosed with lumbosacral stenosis. He was surgically treaeted successfully.
(The image at right depicts the lumbosacral joint, with the L7 vertebra at the top and the sacrum below.)
RETURN TO TOP
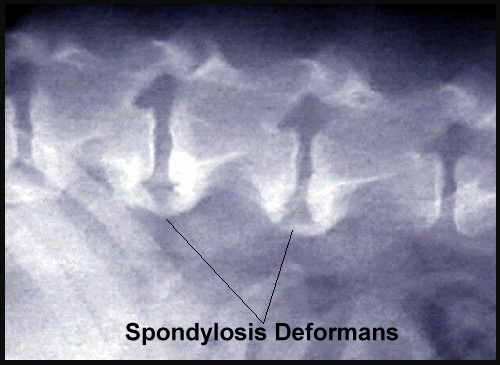
Spondylosis
Spondylosis (spondylosis deformans or vertebral osteophytosis) is a chronic version of disc degeneration in which bony spurs (osteophytes) form on the spine, parallel with the vertebral endplate, and may grow together, connecting one vertebra with another one. There is another bone ossification, called syndesmophyte, that forms in the outer layers of the intervertebral disc. This new bone formation overgrowth perpendicular to vertebral endplate margins is categorized as spondyloarthropathy, which typically becomes noticeable at age 2 years and progresses thereafter. In a March 2016 article, the prevalence of sacroiliac joint erosion or fusion was statistically indistinguishable from that of syndesmophytes in cavaliers.
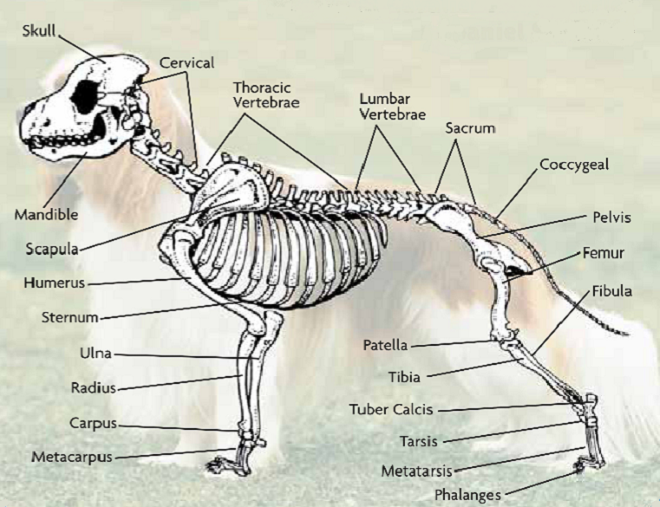 Courtesy of The Dog Channel
Courtesy of The Dog Channel
RETURN TO TOP
Spinal Stroke
A consequential disorder dogs with IVDD is a spinal stroke, also referred to as fibrocartilaginous embolism (FCE) or fibrocartilaginous embolic myelopathy (FCEM). If a fragment of intervertebral disc material should enter a blood vessel, it may block the flow of blood and cause a stroke (infarction) within the spinal cord.
RETURN TO TOP
Symptoms
Intervertebral disc disease (IVDD) can cause a variety of symptoms, ranging
from signs of mild pain to partial or complete paralysis. The most common
symptom is pain, and the most common regions of the spine are the
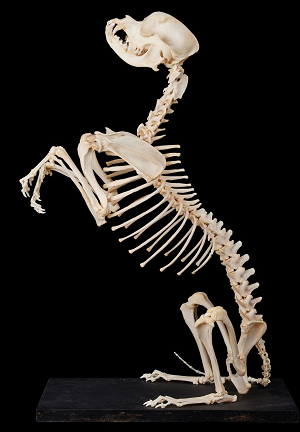 thoracolumbar
(lower back area) and cervical (neck). Observable symptoms
may appear suddenly, intermittently or gradually and could include:
thoracolumbar
(lower back area) and cervical (neck). Observable symptoms
may appear suddenly, intermittently or gradually and could include:
•Stiff or arched back
•Lowered head stance
•Stiff neck
•Lameness
•Dragging one or more legs when walking
•Reluctance to rise
•Yelping unexpectedly when touched or moving
•Spontaneous yelping without any apparent cause
•Fear of being touched, protecting themselves and possibly showing aggression
•Sensitive to movement
•Stilted gait; tentative gait
•Tender or tense abdomen
•Urination difficulties
•Weakness
•Collapse
•Paralysis in one or more limbs
The symptoms may progress from milder ones to more severe ones. (Skeleton at right is of a cavalier King Charles spaniel.)
In the event of a spinal stroke, additional symptoms may include:
•Sudden yelp or cry, followed by inability to move (paralysis)
•Wobbly or unsteady on its feet for several hours.
Other disorders affecting the intervertabal discs may have similiar symptoms. They include, in particular, a bacterial or fungal infection called discospondylitis (diskospondylitis). This disorder is more common among larger breeds, particularly the German shepherd. However, cavaliers have been reported in published studies to have been diagnosed with mycotic discospondylitis, a fungal infection of the discs.
RETURN TO TOP
Diagnosis
A veterinarian’s initial examination of a dog with symptoms of IVDD likely will include physical, orthopedic, and neurologic examinations. The exam may include x-rays (radiographs) and the vet may recommend more extensive tests, such as a myelogram, magnetic resonance imaging (MRI) or computed tomography (CT or CAT scan). A myelogram, CT, or MRI requires that the dog be under general anesthesia.
Neurologic examination, to assess the severity of the disorder and its location along the spine, consists of (1) determining if there is spinal pain; (2) determining if the dog can walk; (3) determining if one side is worse than the other; (4) determining if the pelvic limb spinal reflexes are intact; (5) if unable to walk, determining if there is deep pain perception in the pelvic limbs and tail; (6) if unable to walk, determining if there is a twitch reflex when the skin is pinched (panniculus -- cutaneous trunci -- cut off); and (7) if unable to walk, determining if there is a neurogenic bladder.
X-rays (radiography) are routinely used to initially diagnose cases of suspected IVDD. The use of general anesthesia is recommended by some specialists but rarely is used in such procedures, while sedation is more frequent. X-rays can show narrowing of the space within the affected disc, increased opacity, calcification, and disc material within the vertebral canal. Useful x-rays of the spine, particularly showing it in extension, require specialized knowledge, experience, and supporting equipment (wedges, sandbags, ties). See this YouTube video by Dr. Clare Rusbridge, in which she describes how to get good spinal x-rays. Poor x-rays are a waste of time and money and prevent accurate diagnosis. Placing an awake dog on a flat surface and hoping for the best is not a good practice at all.
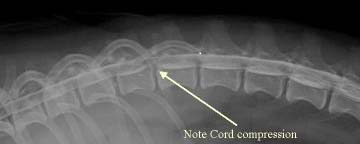 A
myelogram
(right) is an x-ray of the spine, taken after the dog’s spine has been
tapped and cerebrospinal fluid (CSF) has been injected with a dye, to enhance
the view of the spinal cord. The procedure requires a spinal tap, and therefore
the dog must be under general anesthesia. The myelogram should enable the
examiner to locate the affected disc and the precise location of where the disc
is impacting the nerve roots, spinal cord, or surrounding tissues.
However, due to the predominance of syringomyelia in the cavalier King Charles
spaniel, myelography is deemed to be risky in this breed. See this
2005 report.
A
myelogram
(right) is an x-ray of the spine, taken after the dog’s spine has been
tapped and cerebrospinal fluid (CSF) has been injected with a dye, to enhance
the view of the spinal cord. The procedure requires a spinal tap, and therefore
the dog must be under general anesthesia. The myelogram should enable the
examiner to locate the affected disc and the precise location of where the disc
is impacting the nerve roots, spinal cord, or surrounding tissues.
However, due to the predominance of syringomyelia in the cavalier King Charles
spaniel, myelography is deemed to be risky in this breed. See this
2005 report.
 Computed tomography (CT)
is an x-ray technique using digital geometry
processing to generate a three-dimensional image of the inside of an object from
a large series of two-dimensional x-ray images taken around a single axis of
rotation. It is particularly useful when combined with a myelogram, to give the
examiner an independent view of the affected disc, thus eliminating the
likelihood of a misinterpretation due to swelling of the injured spinal cord in
the area of the disc.
Computed tomography (CT)
is an x-ray technique using digital geometry
processing to generate a three-dimensional image of the inside of an object from
a large series of two-dimensional x-ray images taken around a single axis of
rotation. It is particularly useful when combined with a myelogram, to give the
examiner an independent view of the affected disc, thus eliminating the
likelihood of a misinterpretation due to swelling of the injured spinal cord in
the area of the disc.
Magnetic resonance imaging scanning (MRI) is considered to be the "gold standard" for examining herniated discs, because it provides the most detailed images of all aspects of the affected area, including the spinal cord, discs, and nerve roots. MRIs are preferred for cavaliers, due to the breed's high percentage of dogs with syringomyelia. See this 2005 report and this July 2022 ACVIM Consensus Statement.
In an October 2014 study, infrared imaging (thermography) was 90% successful in differentiating between normal dogs and those with Type I thoracolumbar intervertebral disc disease (TLIDD), and 97% successful in identifying the abnormal intervertebral disc space in dogs with TLIVDD.
In a January 2016 study of 46 dogs affected with intervertebral disc (IVD) herniation, including 2 cavalier King Charles spaniels with 11 lesions between them, Egyptian and Japanese researchers compared the accuracy of five different examination procedures (neurological examination*, plain radiography, CT, myelography, and CT myelography) to detect the site of the lesion and the side of the lesion. They found the accuracy rates for determining the site of the lesion as follows: (1) neurological examination: 54.3%; (2) plain radiography: 30.4%; (3) CT: 65.8%; (4) myelography: 84.85%; and (5) CT myelography: 100%. They also reported the accuracy rates for detection of the side of the lesion, as follows: (a) CT: 44,74%; (b) myelography: 54.54%; and (c) CT myelography: 93.9%. They concluded:
"The results of this study suggested that the neurological examination and survey radiography are not reliable for detection of the site of IVD herniation. The accuracy of the CT increases in the chondrodystrophic breeds, which have chronic lesions due to the mineralization of the extruded disc materials. The myelography is considered a valuable tool in the detection of the lesion, especially in the smaller sized dogs. The CT myelography is considered the bset tool in this study for determining the site of IVD herniation and its laterality in dogs."
* This neurological exam consisted of taking blood samples through the recurrent tarsal vein or the jugular vein for hematology and biochemical assay.
Analysis of the CSF may be performed at the time as the diagnostic imaging. For a thorough review of all current methods of diagnosing intervertebral disc diseases, see this October 2020 article.
RETURN TO TOP
Grading IVDD
The severity of intervertebral disc disease (IVDD) is graded on a scale of 1 to 5, as follows:
• Grade 1: Spinal pain only
• Grade 2: Weak but can still walk (ambulatory paraparesis, with or without pain
• Grade 3: Not able to walk (non-ambulatory paraparesis or paraplegia) with or without pain
• Grade 4: Paraplegia, neurogenic bladder, with or without pain
• Grade 5: Paraplegia, neurogenic bladder, and loss of deep pain perception
RETURN TO TOP
DNA Testing
 Researchers at the University of California at Davis (UC Davis)
veterinary genetics laboratory have identified a mutation in the DNA of
a wide variety of breeds of dogs, including cavaliers, which causes chondrodystrophy (CDDY).
The gene is called
Fibroblast growth factor 4 (FGF4),
a developmental signaling gene which normally is expressed at the embryo
stage at specific locations which will develop into the dog's spine and
intervertebral discs. Two retrogenes (DNA genes which have been copied
back from RNA by reverse transcription) of FGF4 have been
located on chromosomes 12 (FGF4L2) and 18 (FGF4L1).
Not all breeds have both retrogenes, and FGF4L2 has been associated with
chondrodystrophy. (FGF4L2 also has caused increasing skull
width in some breeds.)
Researchers at the University of California at Davis (UC Davis)
veterinary genetics laboratory have identified a mutation in the DNA of
a wide variety of breeds of dogs, including cavaliers, which causes chondrodystrophy (CDDY).
The gene is called
Fibroblast growth factor 4 (FGF4),
a developmental signaling gene which normally is expressed at the embryo
stage at specific locations which will develop into the dog's spine and
intervertebral discs. Two retrogenes (DNA genes which have been copied
back from RNA by reverse transcription) of FGF4 have been
located on chromosomes 12 (FGF4L2) and 18 (FGF4L1).
Not all breeds have both retrogenes, and FGF4L2 has been associated with
chondrodystrophy. (FGF4L2 also has caused increasing skull
width in some breeds.)
As the affected young dog matures, chondrodystrophy causes the intervertebral discs to abnormally degenerate at the nucleus pulposus, which is the center of the intervertebral disc that normally provides cushion and flexibility to the back. The end of the degeneration process is to produce a mineralized or calcified disc, which leads to a likelihood of herniation and slippage into the spinal canal. The chondrodystrophic degenerative phenotype may be observed in intervertebral discs as early as 10 weeks of age in CDDY-affected dogs. The researchers at UC Davis have found that the FGF4L2 mutation is dominantly inherited so that dogs with an extra copy of the FGF4 gene, and therefore one copy of the chondrodystrophy mutation, will have degenerative intervertebral disc(s). See this October 2017 article and this June 2019 article and this February 2022 article.
DNA testing is available to determine if a cavalier is chondrodystropic. The UC Davis' veterinary genetics laboratory explains that:
• Dogs with N/N genotype do not have this chondrodystrophy variant and therefore are not predicted to be at increased risk for intervertebral disc disease. They cannot transmit this chondrodystrophy variant to their offspring.
• Dogs with N/CDDY genotype will have leg shortening compared to N/N dogs and intervertebral disc disease, and are at risk for intervertebral disc herniation. They will transmit this CDDY variant to 50% of their offspring. Matings with N/N genotype dogs are predicted to produce 50% shorter-legged puppies at risk for intervertebral disc herniation.
• Dogs with CDDY/CDDY genotype will have leg shortening compared to N/N dogs and intervertebral disc disease, and are at risk for intervertebral disc herniation. If a CDDY/CDDY dog is bred, all of the puppies in the litter will have shorter legs, intervertebral disc disease and will also be at risk for intervertebral disc herniation, regardless of the mate's genotype.
Genetic testing laboratories which test for this mutation causing chondrodystrophy (CDDY) include:
• Embark, Cornell University College of Veterinary Medicine
• GenSol Animal Diagnostics
• Laboklin
• MyDogDNA, Wisdom Panel
• Orivet
• Paw Print Genetics
• Veterinary Genetics Laboratory, University of California - Davis Veterinary Medicine
![]() Watch
this YouTube video to learn how to properly use a swab to obtain DNA from
your dog. See our Genetic Testing webpage for
more information about DNA testing.
Watch
this YouTube video to learn how to properly use a swab to obtain DNA from
your dog. See our Genetic Testing webpage for
more information about DNA testing.
RETURN TO TOP
Related Disorders
Intervertebral disc extrusion (IVDE) is very similar to IVDD in that a disc extrudes from the vertebra, but it is not degenerative. IVDE more often may affect younger cavaliers and be caused by injuries. See this February 2024 article.
Nerve root signature (NRS) is a progressive
lameness or discomfort in a leg due to a disorder of the roots of the
spinal nerve which serve the leg (innervation). It usually is associated
with IVDD and other conditions
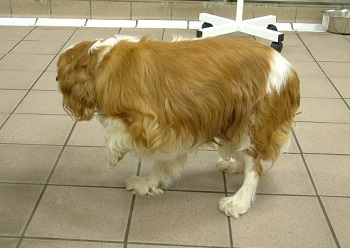 involving
the nerve root(s). It is suspected to be caused by compression,
inflammation, and compromise of the circulatory system around the
affected nerve root. Symptoms include extreme sensitivity to touch,
sharp shooting pain, together with the noted lameness of a single leg.
Lateral disc herniation is the most frequent cause, due to direct
compression upon the nerve root where it emerges from the spinal cord or
inflammation. See this
January 2024 article, in which one cavalier was included in the
study of 51 dogs diagnosed with NRS. (The CKCS in the photo at right
is favoring a limb due to NRS.)
involving
the nerve root(s). It is suspected to be caused by compression,
inflammation, and compromise of the circulatory system around the
affected nerve root. Symptoms include extreme sensitivity to touch,
sharp shooting pain, together with the noted lameness of a single leg.
Lateral disc herniation is the most frequent cause, due to direct
compression upon the nerve root where it emerges from the spinal cord or
inflammation. See this
January 2024 article, in which one cavalier was included in the
study of 51 dogs diagnosed with NRS. (The CKCS in the photo at right
is favoring a limb due to NRS.)
Mycotic discospondylitis is a bacterial or fungal infection causing inflammation of the intervertebral disc and adjacent vertebral endplates This disorder is more common among larger breeds, particularly the German shepherd. However, cavaliers have been reported in published studies to have been diagnosed with mycotic discospondylitis.
RETURN TO TOP
Treatment
- restricted activity
- medications
- surgery
- laser treatment (PLDA)
- injected enzyme
- electromagnetic field treatment (PEMF)
- physiotherapy
- alternative therapies
 Recommended treatment may vary from confinement to surgery and all categories
in between. The form of treatment depends upon the severity of the symptoms, the
myelographic, MRI, or CT Images of the affected area, and the lack of success of
prior, more conservative treatments.
Recommended treatment may vary from confinement to surgery and all categories
in between. The form of treatment depends upon the severity of the symptoms, the
myelographic, MRI, or CT Images of the affected area, and the lack of success of
prior, more conservative treatments.
The main goals of treatment of IVDD are to eliminate the pain and other symptoms, to prevent further disc displacement, and possibly enable the herniated disc to retreat from its displaced position or be resorbed by the body.
-- restricted activity
Typically, for dogs with mild symptoms, the specialist first will prescribe several weeks of very restricted movement, with mostly rest in a cage, to give the spine an opportunity to heal naturally. Such activities as long walks, climbing stairs, and jumping up or down would be strictly off limits.
In the July 2022 ACVIM TL-IVDE* Consensus Statement, the panelists recommend at least 4 weeks of restricted activity to promote healing, ideally in a crate or small room without furniture, no off-leash walking, and no jumping on furniture or access to stairs. For treatment of neuropathic pain, in addition to the medications described below, the panelists recommend hospitalization until the pain is controlled adequately.
*TL-IVDE abbreviates "thoracolumbar intervertebral disc extrusion".If restricted movement alone is not successful, the next option is a combination of medications.
RETURN TO TOP
-- medications
Initially, non-steroidal anti-inflammatory drugs (NSAIDs) including meloxicam (Metacam), firocoxib (Previcox), mavacoxib (Trocoxil), carprofen* (Rimadyl, Quellin), and aspirin will be prescribed.
*Carprofen (Rimadyl, Quellin) may have serious side effects and should not be given without a veterinarian's close guidance and monitoring.
The NSAID usually will be combined with an anticonvulsant (antiepileptic), such as gabapentin (Neurontin, Gabarone) or pregabalin (Lyrica, Accord, Alzain, Lecaent, Milpharm, Prekind, Rewisca, Sandoz, Zentiva).
In an August 2020 article, researchers studied the treatment records of 240 dogs suffering chronic pain due to a variety of diagnosed causes, including osteoarthritis (84.6%), generalized, nonspecific back pain (9.2%), and intervertebral disk disease (7.5%). They report finding that:
"The results from this case series suggest that gabapentin is well-tolerated at much higher doses than what is typically prescribed. Side effects were uncommon, with no clear pattern based on dose, or dog size or age. Therefore, like many other analgesic medications, the efficacy of gabapentin appears patient-specific and should be dosed to effect until side effects are noted or analgesia is achieved.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists recommend the use of NSAIDs for at least 5 to 7 days, provided there are no adverse reactions to the drugs. They also recommend medicating with gabapentin or pregabalin for neuropathic pain, and muscle relaxants such as diazapam or methocarbamol.
In more severe cases, such as those in which the dog's protruding disc(s) have caused injury to the spinal cord, gradual softening and eventual death of cells in the cord may result. This is called progressive myelomalacia (PMM). Anti-inflammatory glucocorticoids (cortisteroids), such as prednisolone (Prelone), methylprednisolone (Medrol, Medrone), and dexamethasone (Decadron, Dexamethasone Intensol, Dexone, Hexadrol), may be prescribed to reduce spinal cord swelling. However, cortisteroids often have undesirable side effects which can interfere with healing and increase the chance of gut perforation or ulceration. Anti-inflammatory doses of glucocorticoids should only be used in medically managed patients under strict cage confinement. The opioid Tramadol is not recommended, as it has been shown to be unreliable in treating dogs and less likely to relieve their pain.
Because of potential for additive adverse side effects (especially gastrointestinal), glucocorticoids and NSAID drugs should never be administered concurrently. Glucocorticoids have serious side effects, such as weight, gait, and skin changes, and harmful suppression of the immune system. Long term use of these drugs is not advised.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists recommend against corticosteroids for routeine use of the acute phase of TL-IVDE, but for the chronic phase, a short course of anti-inflammatory doses of corticosteroids may be of benefit for some dogs.
If muscle spasticity is detected, the vet may administer a muscle relaxant, such as methocarbamol (Robaxin) or guaifenesin (glyceryl guaiacolate). A last resort drug to reduce severe pain would be a narcotic analgesic.
These drugs may also be prescribed following surgery.
RETURN TO TOP
-- surgery
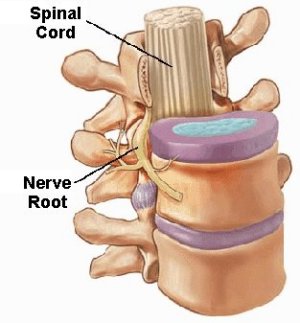 Severely affected dogs, with evidence of spinal cord or nerve root
compression, almost always require some form of decompressive surgery. Spinal
surgery always should be performed only by a board certified veterinary surgeon
or board certified veterinary neurologist using specialized equipment. The spinal cord and nerve roots are
surrounded by the protective bone which forms the vertebral canal.
Severely affected dogs, with evidence of spinal cord or nerve root
compression, almost always require some form of decompressive surgery. Spinal
surgery always should be performed only by a board certified veterinary surgeon
or board certified veterinary neurologist using specialized equipment. The spinal cord and nerve roots are
surrounded by the protective bone which forms the vertebral canal.
The goal of decompressive surgery is to gain access to most of the spinal canal, remove a portion of the bone over the spinal canal, to allow access to the spinal cord, nerve roots, and the herniated disc material, and relieve compression on the spinal cord.
The type of surgical technique may depend upon where the affected disc is located along the spine. Surgeries which remove bone from the upper or back side of the spine are labelled laminectomies. The main decompressive procedures for discs in the neck, called the cervical area, are either a dorsal laminectomy, whereby the surgeon approaches from the back of the neck to reach the vertebrae and discs, or a ventral spondylectomy, or ventral slot procedure, whereby the entry is at the throat, displacing the trachea, esophagus and neuro-vascular trunks to the side to reach the vertebrae and discs.
For discs lower along the spine, in the thoracolumbar area, the procedures are a dorsal laminectomy, followed by a dorsal hemilaminectomy, "hemi" meaning "from the side". A hole is drilled into the vertbral canal, and extruded disc material is removed. A ventral slot, requring approaching the lower spine from the front (ventral) is not a viable option in the thoracolumbar area.
Thoracolumbar lateral corpectomy (TLLC) is a surgical technique for removal of disc material protruding towards the abdomen, with minimal, or ideally no, contact with the spinal cord.
A somewhat controversial surgical procedure, called preventative
fenestration may be recommended. This involves removing the degenerated
center of one or more discs – often up to four to six discs – all through a
 single incision. It is a complex operation with an elevated risk level.
single incision. It is a complex operation with an elevated risk level.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists discuss fenestration at length. They recommend fenestration of the existing herniated disc space during a surgical decompression procedure, to minimize the risk of recurrence at that site. They also advise considering fenestration of adjoining discs which have degenerated but not ruptured, and in some cases, even if the discs are not mineralized. Finally, the suggest that even absent other surgical procedures, fenestration alone could be considered. They point out that the risks associated with fenestration depends upon the site of the affected discs along the spine.
In cases of suspected progressive myelomalacia (PMM), a durotomy is a standard surgical procedure. This involves an incision into the dura, the covering of the spinal cord, to esamine the cord and evaluate its structural integrity to determine if myelomalacia is present or not. The appearance of myelomalacia is oozing of a paste-like substance, together with inflammation, hemorrhaging, and/or fluids causing swelling of the cord.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists observe that each disc extrusion is different and therefore requires unique consideration for the best surgical approach. They note that hemilaminectomy and mini-hemilaminectomy (with or without concurrent fenestration) typically are considered the surgical approaches of choice because of increased ability to access and remove compressive disc material. They state, further:
"Durotomy for dogs with severe neurologic signs may improve outcome and lessen risk of PMM, although further evaluation in a large cohort of dogs is needed. Lateral corpectomy has utility for more chronic or very ventrally located disc extrusions. Fenestration alone, without decompression, is not recommended for dogs with severe (non-ambulatory paraparesis or worse) IVDE. Minimally invasive approaches appear safe and feasible but require further evaluation before they can be routinely adopted."
Disc replacement surgery may be an option. Dr. Filippo Adamo, board
certified veterinary neurologist, has developed replacement disc
implants (the Adamo Spinal Disc - left), which have been shown to be successful
in
 treating disc-associated Wobbler's Syndrome. See his
February 2015 article.
treating disc-associated Wobbler's Syndrome. See his
February 2015 article.
See, also this YouTube video by Dr. Clare Rusbridge on the topic of when to consider surgery for dogs with IVDD.
RETURN TO TOP
-- laser treatment (PLDA)
Percutaneous laser disc ablation (PLDA) is an low-invasive procedure using a HoYAG (Holmium: yttrium-aluminum-garnet) surgical laser which delivers energy at precise locations. It is being used to destroy affected disc matter. First, a spinal needle is inserted into the center of the disc at the intended location. Then the center of the needle (the stylet) is removed and a laser optical fiber is inserted through the hollow center of the needle, and the laser is activated, for less than a minute. See this December 2016 article.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists found the PLDA procedure to be safe and may limit recurrent disc extrusion.
RETURN TO TOP
-- injected enzyme
An experimental procedure is to dissolve the herniated disc by injecting an enzyme called chondroitinase ABC into the disc. The enzymes "digest" the disc but avoid damaging the spinal cord. This process is being tested at Texas A&M University by Dr. Nick Jeffery. The procedure involves anesthesizing the dog and then inserting surgical needles into the affected disc(s) under the guidance of fluoroscopic x-rays. The enzyme is injected into the disc, and it proceeds to dissolve the disc material.
The spinal cord may be affected temporarily, but over the period of about three weeks, dogs being treated with these injecte enzymes reportedly have been able to fully recover and walk and run without support.
Dr. Jeffrey reported the results of this treatment of 50 dogs in this March 2025 article. His report stated that 38 of 40 dogs with intact pain sensation to the hindquarters recovered by a median of 11 days after the intervention, and 4 of 10 dogs without pain sensation recovered. For more information about this procedure, see this link to the Texas A&M's website.
RETURN TO TOP
-- electromagnetic field treatment (PEMF) -- Assisi Loop
Targeted pulsed electromagnetic field (PEMF)
treatments have been studied and used on dogs following
 decompressive
spinal surgery. A device which creates a pulsed electromagnetic field is
placed near the affected area of the dog's body produces a small,
localized electrical field surrounding the dog's affected, inflammed
tissues. This reportedly increases calcium binding by calmodulin, which
binds to constitutive nitric oxide synthase (cNOS), producing nitric
oxide (NO) with a vasodilatory effect encouraging blood-flow, and
limiting inflammation, and increasing bone growth and repair. In an
August 2018 article, North Carolina State veterinary school
researchers reported that a loop PEMF device resulted in evidence of
reduced incision-associated pain in post-IVDD-surgeries and may also
have reduced the extent of spinal cord injury and enhanced gait and
movement function. See also this
March 2019 article. The loop (see image at right) is marketed
as the Assisi Loop to veterinarians and pharmacists. For more
information, see the
Assisi
Animal Health website.
decompressive
spinal surgery. A device which creates a pulsed electromagnetic field is
placed near the affected area of the dog's body produces a small,
localized electrical field surrounding the dog's affected, inflammed
tissues. This reportedly increases calcium binding by calmodulin, which
binds to constitutive nitric oxide synthase (cNOS), producing nitric
oxide (NO) with a vasodilatory effect encouraging blood-flow, and
limiting inflammation, and increasing bone growth and repair. In an
August 2018 article, North Carolina State veterinary school
researchers reported that a loop PEMF device resulted in evidence of
reduced incision-associated pain in post-IVDD-surgeries and may also
have reduced the extent of spinal cord injury and enhanced gait and
movement function. See also this
March 2019 article. The loop (see image at right) is marketed
as the Assisi Loop to veterinarians and pharmacists. For more
information, see the
Assisi
Animal Health website.
RETURN TO TOP
-- physiotherapy
Physiotherapy usually immediately follows surgeries and in the case of spinal stroke. It includes simple exercise programs such as walking the dog with support, leg lifts, using balancing platforms, and water therapy, all to improve joint position sense and core strength.
In the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists recommend basic physical rehabilitation exercises, such as passive range of motion exercises and massage, as an additional treatment of medically treated dogs, combined with restricted activity for at least 4 weeks, followed by increased levels of physical activity.
RETURN TO TOP
-- alternative therapies
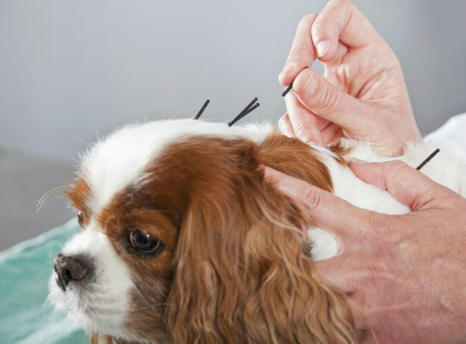 In some cases, non-traditional therapies such as holistic healing,
especially homeopathy and acupuncture (right), may be useful alternatives to conventional
medicine and surgery.
In some cases, non-traditional therapies such as holistic healing,
especially homeopathy and acupuncture (right), may be useful alternatives to conventional
medicine and surgery.
Homeopathic remedies, when prescribed by licensed veterinarians who, in addition to their veterinary medical education, are further educated and trained and certified in holistic veterinary modalites, have successfully treated disc disorders. Such remedies have included Rhus tox, Pulsatilla, and a few others.
Acupuncture, and in particular, electro-acupunture, has been successful for dogs which have signs of pain alone, or only mild neurologic deficits. In this September 2023 article, the recovery rate of acupuncture treatments of 94 dogs of 24 breeds was 79.78%.
Oddly, in the July 2022 ACVIM TL-IVDE Consensus Statement, the panelists recommend against acupunture treatment as an alternative to surgery, but they do not comment on its use apart from as a substitute for surgery.
Stem cell treatments, also called mesenchymal stem cell transplantation, has been the subject of research with results indicating some success in treating dogs with IVDD. For instance, in this October 2009 article, it concluded:
"Autologous adipose tissue derived stem and regenerative cells, as used in this disc injury model, were effective in promoting disc regeneration, as evidenced by disc matrix production and overall disc morphology."
See also this January 2008 article and this October 2010 article.
RETURN TO TOP
Research News
January 2025:
Cavaliers ranked fourth in prevalence of owner-reported
intervertebral disc disease among 43,517 dogs in USA.
 In
a
January 2025 article of a study of 43,517 dogs in the USA during
2020-2022, researchers Crystal Wee (right) and Darren Z. Nin
reported that among owner-reported cases of intervertebral disc disease
(IVDD), the breeds with increased odds of owner-reported IVDD were
French bulldogs, Dachshunds, beagles, cavalier King Charles spaniels,
and Newfoundlands in that order.
In
a
January 2025 article of a study of 43,517 dogs in the USA during
2020-2022, researchers Crystal Wee (right) and Darren Z. Nin
reported that among owner-reported cases of intervertebral disc disease
(IVDD), the breeds with increased odds of owner-reported IVDD were
French bulldogs, Dachshunds, beagles, cavalier King Charles spaniels,
and Newfoundlands in that order.
EDITOR'S NOTE: Expecting accurate diagnoses based upon dog owners' surveys of their dogs suffering pain can be iffy at best. So, whether or not cavaliers really are ranked 4th is not particularly reliable from a scientific standpoint.
February 2024:
Cavalier with extruded disc in its neck is healed without
surgery.
 In
a
February 2024 case study, two UK clinicians (Michelle du Toit
[right], Neringa Alisauskaite) report a 4-year-old cavalier King
Charles spaniel diagnosed with a painful condition due to a disc
extruding from his spine, in a case of
intervertebral disc
extrusion (IVDE) in the neck (cervical) region of the spine (at
C7-T1). The dog's symptoms included hyperesthesia (extreme pain and
sensitivity), a stiff gait, low head carriage, and reluctance to turn
the neck or lift the head. This condition was distinguished from
degenerative intervertebral disc disease (IVDD) in that it is not
considered to be degenerative. MRI was performed, and extruded disc
material was observed at the C7-T1 location on the spine, resulting in
50% reduction in the area of the vertebral canal and severe compression
of the spinal cord. The disc material also was compressing the C8 nerve
roots. (See MRI image below.) Surgical decompression was an
option, but the owner chose a more conservative therapy consisting of
exercise restriction and medication for a period of 4 to 8 weeks.
Initially, the dog was hospitalized for 8 days, followed by being
confined to his cage with only brief walks on leads.
In
a
February 2024 case study, two UK clinicians (Michelle du Toit
[right], Neringa Alisauskaite) report a 4-year-old cavalier King
Charles spaniel diagnosed with a painful condition due to a disc
extruding from his spine, in a case of
intervertebral disc
extrusion (IVDE) in the neck (cervical) region of the spine (at
C7-T1). The dog's symptoms included hyperesthesia (extreme pain and
sensitivity), a stiff gait, low head carriage, and reluctance to turn
the neck or lift the head. This condition was distinguished from
degenerative intervertebral disc disease (IVDD) in that it is not
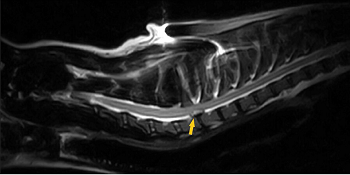
considered to be degenerative. MRI was performed, and extruded disc
material was observed at the C7-T1 location on the spine, resulting in
50% reduction in the area of the vertebral canal and severe compression
of the spinal cord. The disc material also was compressing the C8 nerve
roots. (See MRI image below.) Surgical decompression was an
option, but the owner chose a more conservative therapy consisting of
exercise restriction and medication for a period of 4 to 8 weeks.
Initially, the dog was hospitalized for 8 days, followed by being
confined to his cage with only brief walks on leads.
 Treatment
consisted of physical therapy and medication (gabapentin, amantadine,
paracetamol, and only when necessary, either methadone or
buprenorphine). The cavalier had a couple of relapses of extreme pain
and sensitivity and subsequently displayed right rear leg lameness. MRI
after 4 months showed another disc extruding at L5-L6, diagnosed as
degenerative IVDE (called "foraminal"), requiring surgery. However, the
MRI showed that the C7-T1 disc had returned to its proper position.
Treatment
consisted of physical therapy and medication (gabapentin, amantadine,
paracetamol, and only when necessary, either methadone or
buprenorphine). The cavalier had a couple of relapses of extreme pain
and sensitivity and subsequently displayed right rear leg lameness. MRI
after 4 months showed another disc extruding at L5-L6, diagnosed as
degenerative IVDE (called "foraminal"), requiring surgery. However, the
MRI showed that the C7-T1 disc had returned to its proper position.
February 2023:
Herniated discs may be dissolved by injecting chondroitinase ABC
enzyme into them.
 An
experimental procedure is to dissolve the herniated disc by injecting an
enzyme called chondroitinase ABC into the disc. The enzymes "digest" the
disc but avoid damaging the spinal cord. This process is being tested at
Texas A&M University by veterinary neurologist Dr. Nick Jeffery
(right). The procedure involves anesthesizing the dog and then
inserting surgical needles into the affected disc(s) under the guidance
of fluoroscopic x-rays. The enzyme is injected into the disc, and it
proceeds to dissolve the disc material. The spinal cord may be affected
temporarily, but over the period of about three weeks, dogs being
treated with these injected enzymes reportedly have been able to fully
recover and walk and run without support. See this
March 2025 article for details.
An
experimental procedure is to dissolve the herniated disc by injecting an
enzyme called chondroitinase ABC into the disc. The enzymes "digest" the
disc but avoid damaging the spinal cord. This process is being tested at
Texas A&M University by veterinary neurologist Dr. Nick Jeffery
(right). The procedure involves anesthesizing the dog and then
inserting surgical needles into the affected disc(s) under the guidance
of fluoroscopic x-rays. The enzyme is injected into the disc, and it
proceeds to dissolve the disc material. The spinal cord may be affected
temporarily, but over the period of about three weeks, dogs being
treated with these injected enzymes reportedly have been able to fully
recover and walk and run without support. See this
March 2025 article for details.
July 2022:
ACVIM issues a consensus statement on canine thoracolumbar
intervertebral disc extrusion.
 In
a
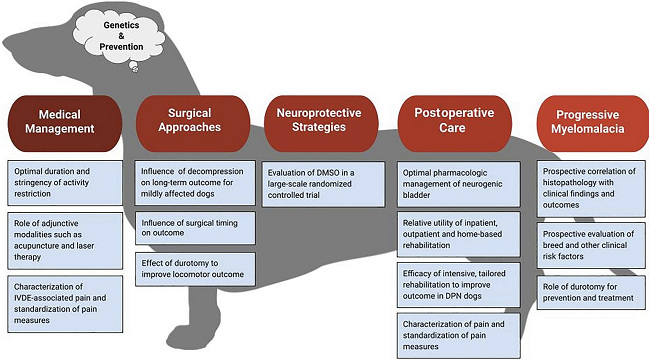
July 2022 article, the ACVIM published a consensus statement by a a
panel of eight specialists (Sarah A. Moore, Natasha J. Olby, Brigitte
Brisson, Joe Fenn, Thomas Flegel, Gregg Kortz, Melissa Lewis, Andrea
Tipold), regarding the diagnosis and management of acute canine
thoracolumbar intervertebral disc extrusion. While cavaliers are not at
the top of the list of affected breeds, disc extrusions are common in
the CKCS breed, mainly because the breed suffers from chondrodystrophy
(CDDY), a congenital disorder which originates in the embryo due to a
mutation of a particular gene and then progresses into Hansen type I
intervertebral disc extrusion as the dog ages. In the Consensus
Statement, the panelists provide a series of recommendations regarding
treatment options, medications versus surgeries, types of surgeries and
post-operative care. The panel's advice is too detailed to list here,
and has been included throughout the main sections of this webpage. See
also this chart:
In
a
July 2022 article, the ACVIM published a consensus statement by a a
panel of eight specialists (Sarah A. Moore, Natasha J. Olby, Brigitte
Brisson, Joe Fenn, Thomas Flegel, Gregg Kortz, Melissa Lewis, Andrea
Tipold), regarding the diagnosis and management of acute canine
thoracolumbar intervertebral disc extrusion. While cavaliers are not at
the top of the list of affected breeds, disc extrusions are common in
the CKCS breed, mainly because the breed suffers from chondrodystrophy
(CDDY), a congenital disorder which originates in the embryo due to a
mutation of a particular gene and then progresses into Hansen type I
intervertebral disc extrusion as the dog ages. In the Consensus
Statement, the panelists provide a series of recommendations regarding
treatment options, medications versus surgeries, types of surgeries and
post-operative care. The panel's advice is too detailed to list here,
and has been included throughout the main sections of this webpage. See
also this chart:
August 2020:
Colorado State Univ. researchers find gabapentin is
well-tolerated at high dosages for dogs in chronic pain.
 In
an
August 2020 article, a team of Colorado State University researchers
(Lily V Davis, Peter W Hellyer, Robin A Downing, Lori R Kogan [right])
studied the treatment records of 240 dogs suffering chronic pain due to
a variety of diagnosed causes, including osteoarthritis (84.6%),
generalized, nonspecific back pain (9.2%), intervertebral disk disease
(7.5%), degenerative myelopathy (4.6%), and 56.67% not having a
definitive anatomical cause for their pain. They
report finding that:
In
an
August 2020 article, a team of Colorado State University researchers
(Lily V Davis, Peter W Hellyer, Robin A Downing, Lori R Kogan [right])
studied the treatment records of 240 dogs suffering chronic pain due to
a variety of diagnosed causes, including osteoarthritis (84.6%),
generalized, nonspecific back pain (9.2%), intervertebral disk disease
(7.5%), degenerative myelopathy (4.6%), and 56.67% not having a
definitive anatomical cause for their pain. They
report finding that:
"The results from this case series suggest that gabapentin is well-tolerated at much higher doses than what is typically prescribed. Side effects were uncommon, with no clear pattern based on dose, or dog size or age. Therefore, like many other analgesic medications, the efficacy of gabapentin appears patient-specific and should be dosed to effect until side effects are noted or analgesia is achieved.
October 2019:
UK neurologists report successful surgery on a young cavalier
for congenital vertebral compression of the spinal cord.
 In
an October 2019 case study report, a team of UK neurology clinicians
(Fabio Stabile [right], Robert Brash, Luisa De Risio) report
the successful surgery on a 2-year-old female cavalier suffering from
painful spinal cord compression, diagnosed as hyperplasia of the caudal
vertebral articular process (CVAP). This is a congenital disorder
different from degenerative joint disease. The dog underwent a T12–T13
dorsal laminectomy and spinal cord decompression by removal of the
hyperplastic CVAP of T12. The dog was released 3 days after surgery for
4 weeks of restricted exercise and treatment with meloxicam and
gabapentin. Over the following 6 years of follow-up examinations, the
CKCS progressively improved to the point of full physical recovery.
In
an October 2019 case study report, a team of UK neurology clinicians
(Fabio Stabile [right], Robert Brash, Luisa De Risio) report
the successful surgery on a 2-year-old female cavalier suffering from
painful spinal cord compression, diagnosed as hyperplasia of the caudal
vertebral articular process (CVAP). This is a congenital disorder
different from degenerative joint disease. The dog underwent a T12–T13
dorsal laminectomy and spinal cord decompression by removal of the
hyperplastic CVAP of T12. The dog was released 3 days after surgery for
4 weeks of restricted exercise and treatment with meloxicam and
gabapentin. Over the following 6 years of follow-up examinations, the
CKCS progressively improved to the point of full physical recovery.
January 2016:
A study
including cavaliers finds CT myelography is 100% accurate in detecting
the sites of intervertebral disc herniation lesions.
 In a
January 2016 study of 46 dogs affected with intervertebral disc
(IVD) herniation, including 2 cavalier King Charles spaniels with 11
lesions between them, Egyptian and Japanese researchers (Mohammed
Abdel-Hakiem [right], Masaaki Katayama, Ahmed Saleh, Haroun
Youssef, Yasuhiko Okamura, Yuji Uzuka) compared the
accuracy of five different examination procedures (neurological
examination*, plain radiography, CT,
myelography**, and CT myelography) to
detect the site of the lesion and the side of the lesion.
In a
January 2016 study of 46 dogs affected with intervertebral disc
(IVD) herniation, including 2 cavalier King Charles spaniels with 11
lesions between them, Egyptian and Japanese researchers (Mohammed
Abdel-Hakiem [right], Masaaki Katayama, Ahmed Saleh, Haroun
Youssef, Yasuhiko Okamura, Yuji Uzuka) compared the
accuracy of five different examination procedures (neurological
examination*, plain radiography, CT,
myelography**, and CT myelography) to
detect the site of the lesion and the side of the lesion.
They found the accuracy rates for determining the site of the lesion as follows: (1) neurological examination: 54.3%; (2) plain radiography: 30.4%; (3) CT: 65.8%; (4) myelography: 84.85%; and (5) CT myelography: 100%. They also reported the accuracy rates for detection of the side of the lesion, as follows: (a) CT: 44,74%; (b) myelography: 54.54%; and (c) CT myelography: 93.9%. They concluded:
"The results of this study suggested that the neurological examination and survey radiography are not reliable for detection of the site of IVD herniation. The accuracy of the CT increases in the chondrodystrophic breeds, which have chronic lesions due to the mineralization of the extruded disc materials. The myelography is considered a valuable tool in the detection of the lesion, especially in the smaller sized dogs. The CT myelography is considered the bset tool in this study for determining the site of IVD herniation and its laterality in dogs."
* The
neurological exam consisted of taking blood samples through the
recurrent tarsal vein or the jugular vein for hematology and biochemical
assay.
** A myelogram
consists of tapping the dog’s spine and injecting the cerebrospinal
fluid (CSF) with a dye, to enhance the view of the spinal cord. The
procedure requires a spinal tap, and therefore the dog must be under
general anesthesia.
EDITOR'S NOTE: In a 2005 report, myelography has been deemed too risky to conduct in cavaliers, due to the predominance of syringomyelia in the breed.
 February 2015: NC State
research team finds 4-Aminopyridine (4-AP and t-butyl) enable paralyzed
dogs to walk, wag tails. In a
December 2014 report, North Carolina State's Dr. Natasha Olby
(right) and
her a team found that two potassium channel antagonists, 4-Aminopyridine
(4-AP) and N- (4-pyridine) t-butyl carbamate derivative of 4-AP (T-BOC),
enabled dogs with acute spinal cord injuries to walk and wag their
tails, by restoring the ability to conduct nerve impulses and improving
function in the injured animal.
February 2015: NC State
research team finds 4-Aminopyridine (4-AP and t-butyl) enable paralyzed
dogs to walk, wag tails. In a
December 2014 report, North Carolina State's Dr. Natasha Olby
(right) and
her a team found that two potassium channel antagonists, 4-Aminopyridine
(4-AP) and N- (4-pyridine) t-butyl carbamate derivative of 4-AP (T-BOC),
enabled dogs with acute spinal cord injuries to walk and wag their
tails, by restoring the ability to conduct nerve impulses and improving
function in the injured animal.
December 2014:
New drug lets paralyzed rats move after spinal cord injuries.
 A team of US researchers, led by Dr. Bradley Lang of Case Western
Reserve University School of Medicine (right), state in a
December 2014 report
that they designed a drug, intracellular sigma peptide (ISP), which they
injected beneath the skin of paralyzed rats near the spinal injury site.
After spinal cord injury, axons try to cross the injury site and
reconnect with other cells but are stymied by scarring that forms after
the injury. Previous studies suggested their movements are blocked when
the protein tyrosine phosphatase sigma (PTP sigma), an enzyme found in
axons, interacts with chondroitin sulfate proteoglycans, a class of
sugary proteins that fill the scars. Injected ISP blocked the enzyme and
facilitated the drug’s entry into the brain and spinal cord, partially
restoring axon growth and improving movements and bladder functions.
A team of US researchers, led by Dr. Bradley Lang of Case Western
Reserve University School of Medicine (right), state in a
December 2014 report
that they designed a drug, intracellular sigma peptide (ISP), which they
injected beneath the skin of paralyzed rats near the spinal injury site.
After spinal cord injury, axons try to cross the injury site and
reconnect with other cells but are stymied by scarring that forms after
the injury. Previous studies suggested their movements are blocked when
the protein tyrosine phosphatase sigma (PTP sigma), an enzyme found in
axons, interacts with chondroitin sulfate proteoglycans, a class of
sugary proteins that fill the scars. Injected ISP blocked the enzyme and
facilitated the drug’s entry into the brain and spinal cord, partially
restoring axon growth and improving movements and bladder functions.
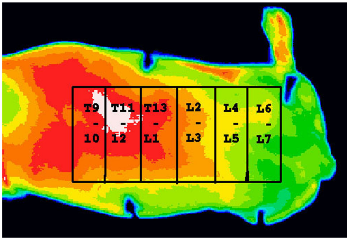 November 2014:
Infrared imaging study finds 90% success in identifying dogs with Type I
intervertebral disk disease. In
an October 2014 study of 70
dogs by a US team of researchers led by Dr. Dominic J. Marino, they
found that medical infrared imaging (thermography) was 90% successful in
differentiating between normal dogs and those with Type I thoracolumbar
intervertebral disk disease (TLIDD), and 97% successful in identifying
the abnormal intervertebral disc space in dogs with TLIVDD.
November 2014:
Infrared imaging study finds 90% success in identifying dogs with Type I
intervertebral disk disease. In
an October 2014 study of 70
dogs by a US team of researchers led by Dr. Dominic J. Marino, they
found that medical infrared imaging (thermography) was 90% successful in
differentiating between normal dogs and those with Type I thoracolumbar
intervertebral disk disease (TLIDD), and 97% successful in identifying
the abnormal intervertebral disc space in dogs with TLIVDD.
November
2012: German researchers assess effect of gabapentin on post-operative
pain after
 intervertebral disc surgery. In
a November 2012
report in Veterinary Anaesthesia and Analgesia, involving 63 dogs, German
neurologists compared the pain-relief value of gabapentin when added to opioid
analgesia. They concluded that gabapentin administered orally twice a day "did
not result in a detectable reduction in pain behaviour compared to background
opioid analgesia alone." However, they recommend further studies to determine if
the results were related to effective background analgesia or an ineffective
dose of gabapentin.
intervertebral disc surgery. In
a November 2012
report in Veterinary Anaesthesia and Analgesia, involving 63 dogs, German
neurologists compared the pain-relief value of gabapentin when added to opioid
analgesia. They concluded that gabapentin administered orally twice a day "did
not result in a detectable reduction in pain behaviour compared to background
opioid analgesia alone." However, they recommend further studies to determine if
the results were related to effective background analgesia or an ineffective
dose of gabapentin.
July 2012: NC State studies potassium channel antagonists to treat spinal cord injuries. North Carolina State's Dr. Natasha Olby leads a team evaluating two potassium channel antagonists, 4-Aminopyridine (4-AP) and N- (4-pyridine) t-butyl carbamate derivative of 4-AP (T-BOC) as treatments of dogs with acute spinal cord injuries. Potassium channel antagonists block potassium channels on this exposed tissue, restoring its ability to conduct nerve impulses and improving function in the injured animal. Read the details here.
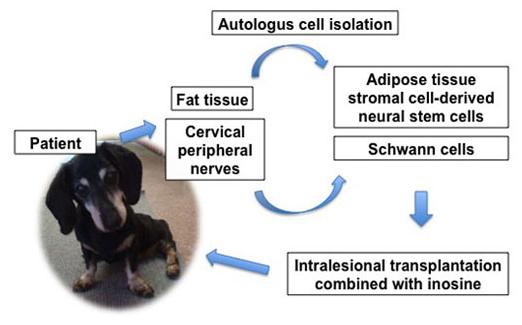
February 2012: NC State needs dogs for stem cell research of spinal cord injuries. Dr. Natasha Olby of North Carolina State's veterinary college is leading a clinical trial in which stem cells are injected into dogs' herniated discs. According to Dr. Olby, even in the case of severe spinal cord injury all may not be lost in terms of spinal cord function – there may still be salvageable, living nerves and nerve fibers, or axons, bridging the site of the injury that could still transmit signals if they had a little help. Dr. Olby's team target surviving nerves and axons that are still crossing the site of the injury and seek to restore their conductivity.
![]() Often, these damaged nerves have lost the myelin sheath, fatty material that
coats axons and allows them to conduct signals. Dr. Olby wants to restore the
myelin sheath to these surviving axons by taking fat cells from the patient and
turning them into stem cells that can be combined with nerve cells and injected
into the site of the damage, regrowing the sheath. Even though she is still in
the early stages of a randomized clinical trial, the results thus far are
reportedly encouraging. Her team still need candidate dogs for this study.
Watch a YouTube video of Dr. Olby explaining this research project here.
Often, these damaged nerves have lost the myelin sheath, fatty material that
coats axons and allows them to conduct signals. Dr. Olby wants to restore the
myelin sheath to these surviving axons by taking fat cells from the patient and
turning them into stem cells that can be combined with nerve cells and injected
into the site of the damage, regrowing the sheath. Even though she is still in
the early stages of a randomized clinical trial, the results thus far are
reportedly encouraging. Her team still need candidate dogs for this study.
Watch a YouTube video of Dr. Olby explaining this research project here.
The project's inclusion criteria include:
 • Dogs must have suffered a thoracolumbar spinal cord injury at least 3
months previously from which they have failed to recover either motor or sensory
function in their hind limbs.
• Dogs must have suffered a thoracolumbar spinal cord injury at least 3
months previously from which they have failed to recover either motor or sensory
function in their hind limbs.
• Dogs with only limited or no
motor function in their hind limbs will be admitted – this will be determined at
the first evaluation by the investigators.
• Dogs will have to be
videotaped when walking on a treadmill and so we can only include dogs that will
tolerate working with the investigators on the treadmill.
• Dogs must also be in good
health other than their spinal cord injury: dogs with urinary tract infections
will not be able to start the study until the infection is treated.
• The owner must be willing to
come to the hospital with their dog once a week for the first month of the trial
and then once a month for the remainder of the trial.
For more information, click here.
RETURN TO TOP
Related Links
RETURN TO TOP
Veterinary Resources
Intervertebral Disk Disease, Chapter 62, Textbook of Small Animal Orthopedics. Andy Shores. 1982; U. Penn CAL small animal orthopedics.
Spondylosis Deformans, Chapter 61, Textbook of Small Animal Orthopedics. Joseph P. Morgan, Darryl N. Biery . 1982; U. Penn CAL small animal orthopedics.
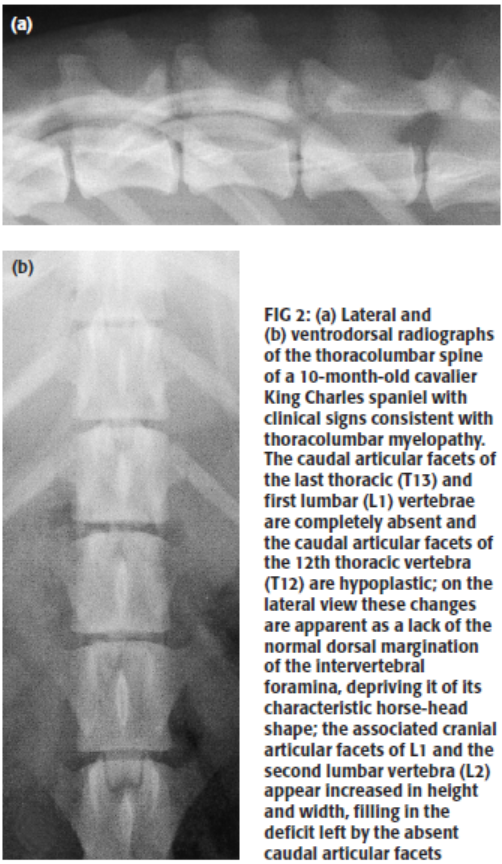 Dysplasia
of the caudal vertebral articular facets in four dogs: results of
radiographic, myelographic and magnetic resonance imaging investigations.
J. Penderis, T. Schwarz, J. F. McConnell, L. S. Garosi, C. E. Thomson, R.
Dennis. Vet. Rec. May 2005;156:601–5. Quote: Congenital anomalies of the
vertebral column associated with aberrations of one of the primary vertebral
ossification centres have been frequently described in the veterinary
literature, but clinically significant abnormalities of secondary vertebral
ossification centres, particularly involving the caudal articular processes,
are much less frequently reported. This paper describes three dogs with
aplasia [two German shepherds and a 10-month-old cavalier King
Charles spaniel] and one dog with hypoplasia of the caudal
vertebral articular processes. Thoracolumbar spinal cord compression and
ataxia was evident in the three dogs with aplasia but no clinical signs were
evident in the dog with hypoplasia. The radiographic appearance was similar
in all four cases, with aplasia or hypoplasia of the caudal articular facets
at one or more intervertebral joints in the thoracolumbar region. Bone
proliferation was evident secondary to an associated degenerative joint
disease. Compensatory hyperplasia of the adjacent cranial articular facets
and ligamentum flavum protruded into the vertebral canal, resulting in a
compressive myelopathy observed by myelography and magnetic resonance
imaging. ... The results of this study show that congenital abnormalities of
the caudal articular facets occur in dogs, demonstrate the typical imaging
findings and suggest that the total absence of the caudal articular facets
may result in neurological deficits.
Dysplasia
of the caudal vertebral articular facets in four dogs: results of
radiographic, myelographic and magnetic resonance imaging investigations.
J. Penderis, T. Schwarz, J. F. McConnell, L. S. Garosi, C. E. Thomson, R.
Dennis. Vet. Rec. May 2005;156:601–5. Quote: Congenital anomalies of the
vertebral column associated with aberrations of one of the primary vertebral
ossification centres have been frequently described in the veterinary
literature, but clinically significant abnormalities of secondary vertebral
ossification centres, particularly involving the caudal articular processes,
are much less frequently reported. This paper describes three dogs with
aplasia [two German shepherds and a 10-month-old cavalier King
Charles spaniel] and one dog with hypoplasia of the caudal
vertebral articular processes. Thoracolumbar spinal cord compression and
ataxia was evident in the three dogs with aplasia but no clinical signs were
evident in the dog with hypoplasia. The radiographic appearance was similar
in all four cases, with aplasia or hypoplasia of the caudal articular facets
at one or more intervertebral joints in the thoracolumbar region. Bone
proliferation was evident secondary to an associated degenerative joint
disease. Compensatory hyperplasia of the adjacent cranial articular facets
and ligamentum flavum protruded into the vertebral canal, resulting in a
compressive myelopathy observed by myelography and magnetic resonance
imaging. ... The results of this study show that congenital abnormalities of
the caudal articular facets occur in dogs, demonstrate the typical imaging
findings and suggest that the total absence of the caudal articular facets
may result in neurological deficits.
Neurological diseases of the Cavalier King Charles spaniel. C. Rusbridge. J.Sm.Ani.Pract. 2005; 46:265–272. Quote: "The CKCS is a chondrodystrophic-type breed and as such is prone to Hansen type I disc extrusions. The most common clinical sign is spinal pain, with or without paresis. Disc extrusion is uncommon in dogs younger than two years of age. Survey radiographs may indicate possible sites of disc extrusion by identifying a narrowed intervertebral disc space, foramen or joint spaces, or by finding calcified disc material within the vertebral canal. For confirmation of the diagnosis, further imaging such as myelography or magnetic resonance imaging (MRI) is required. MRI is preferred because of the tendency for CKCSs to have syringomyelia and subsequently a small cisterna magnum and subarachnoid space, presenting an increased risk of intrathecal spinal needle placement. Lumbar, as well as cisternal, myelography is risky in this breed. Management of disc disease may be medical (analgesia and exercise restriction for at least four weeks) or surgical. Surgical management is preferred for dogs with significant paresis or paralysis. For the optimum chance of return of function, dogs without deep pain perception should have decompressive surgery performed within 24 hours of loss of function."
Conservative Management of Chondrodystrophic Dogs with Thoracolumbar Intervertebral Disc Disease. Laurie Edge-Hughes. CHAP Newsletter. December 2007;4–6.
Transplantation of Mesenchymal Stem Cells in a Canine Disc Degeneration Model. Akihiko Hiyama, Joji Mochida, Toru Iwashina, Hiroko Omi, Takuya Watanabe, Kenji Serigano, Futoshi Tamura,Daisuke Sakai. J. Orthopaedic Res. January 2008;26(5):589-600. Quote: Transplantation of mesenchymal stem cells (MSCs) is effective in decelerating disc degeneration in small animals; much remains unknown about this new therapy in larger animals or humans. Fas-ligand (FasL), which is only found in tissues with isolated immune privilege, is expressed in IVDs, particularly in the nucleus pulposus (NP). Maintaining the FasL level is important for IVD function. This study evaluated whether MSC transplantation has an effect on the suppression of disc degeneration and preservation of immune privilege in a canine model of disc degeneration. Mature beagles were separated into a normal control group (NC), a MSC group, and the disc degeneration (nucleotomy-only) group. In the MSC group, 4 weeks after nucleotomy, MSCs were transplanted into the degeneration-induced discs. The animals were followed for 12 weeks after the initial operation. Subsequently, radiological, histological, biochemical, immunohistochemical, and RT-PCR analyses were performed. MSC transplantation effectively led to the regeneration of degenerated discs. FACS and RT-PCR analyses of MSCs before transplantation demonstrated that the MSCs expressed FasL at the genetic level, not at the protein level. GFP-positive MSCs detected in the NP region 8 weeks after transplantation expressed FasL protein. The results of this study suggest that MSC transplantation may contribute to the maintenance of IVD immune privilege by the differentiation of transplanted MSCs into cells expressing FasL.
Intervertebral Disc Disease (IVDD). Patty Khuly. Quote: "The more typical, Type I IVDD is common in the dachshund along with many other chondrodystrophic breeds of dogs including the basset hound, beagle, French bulldog, Lhasa apso, Pekingese, pomeranian, shih tzu, and Welsh corgi. Cocker spaniels, Cavalier King Charles spaniels and other semi-chondrodystrophic breeds are also predisposed."
Intervertebral Disc Repair Using Adipose Tissue-Derived Stem and Regenerative Cells: Experiments in a Canine Model. Ganey, Timothy, Hutton, William C., Moseley, Timothy, Hedrick, Mark, Meisel, Hans-Joerg. Spine. October 2009;34(21):2297-2304. Quote: Study Design: Therapeutic treatment of intervertebral disc repair using cells. Objective: The goal of the study was to test the hypothesis that repair of a damaged disc is possible using autologous adipose tissue derived stem and regenerative cells (ADRCs). Summary of Background Data: Degradation resulting from either acute or chronic repetitive disc injury leads to disc degeneration. However, if a damaged disc could be repaired in the early stages, before the onslaught of degradation, then the disc degeneration process may be slowed down. Methods: Twelve dogs underwent a partial nucleotomy at 3 lumbar levels (L3–L4, L4–L5, and L5–L6); adjacent levels served as nonoperated controls. The animals (or discs) were allowed to recover from the surgery for 6 weeks. At that time subcutaneous adipose tissue was harvested and ADRCs were isolated. The 3 experimental discs that had undergone a partial nucleotomy were randomized to receive: (1) ADRCs in hyaluronic acid carrier (Cells/HA); (2) HA only; or (3) No Intervention. Assessments of the 3 experimental discs plus the 2 adjacent untouched discs were made using MRI, radiography, histology, and biochemistry. The animals were killed at 6 months and at 12 months. Results: Repair in this study was specifically demonstrated through histology and biochemical analysis. Disc levels receiving ADRCs more closely resembled the healthy controls as evidenced in matrix translucency, compartmentalization of the anulus, and in cell density within the nucleus pulposus. Matrix analysis for Type-II collagen and aggrecan demonstrated evidence of a statistically better regenerative stimulation to the disc provided by ADRCs when compared to either the HA only or no intervention treatments. Conclusion: Autologous adipose tissue derived stem and regenerative cells, as used in this disc injury model, were effective in promoting disc regeneration, as evidenced by disc matrix production and overall disc morphology.
Presumptive exercise-associated peracute thoracolumbar disc extrusion in 48 dogs. W. M. McKee, C. J. Downes, J. J. Pink, T. J. Gemmill. Vet.Rec. April 2010; 166:523-528. Quote: "Forty-eight dogs [including a cavalier King Charles spaniel] were diagnosed with presumptive exercise-associated peracute thoracolumbar disc extrusion. The median age was seven years (range two to 11 years), and median bodyweight was 23 kg (range 10 to 41 kg). The duration of signs before presentation ranged from 0.5 to four days. Twenty-nine dogs were non-ambulatory, of which 17 were incontinent and two had lost pain perception. Pelvic limbs were hyporeflexic or areflexic in 11 dogs. Intervertebral disc narrowing was evident on radiographs in 44 dogs. Myelography demonstrated a small, extradural space-occupying lesion dorsal to an intervertebral disc between T11-12 and L3-4 with adjacent spinal cord swelling. Forty-six dogs were treated non-surgically, one was euthanased and one was managed by hemilaminectomy (and subsequently euthanased). Follow-up information was available for 46 dogs 1.5 to 55 months after injury (median 22 months) showing that pelvic limb function had improved in all cases and all non-ambulatory dogs had regained the ability to walk. Six dogs remained faecally incontinent, and one dog remained urinarily and faecally incontinent."
Effect of cell number on mesenchymal stem cell transplantation in a canine disc degeneration model. Kenji Serigano, Daisuke Sakai, Akihiko Hiyama, Futoshi Tamura, Masahiro Tanaka, Joji Mochida. J. Orthopaedic Res. October 2010;28(10):1267-1275. Quote: Transplantation of mesenchymal stem cells (MSCs) inhibits the progression of disc degeneration in animal models. We know of no study to determine the optimal number of cells to transplant into the degenerated intervertebral disc (IVD). To determine the optimal donor cell number for maximum benefit, we conducted an in vivo study using a canine disc degeneration model. Autologous MSCs were transplanted into degenerative discs at 105, 106, or 107 cells per disc. The MSC-transplanted discs were evaluated for 12 weeks using plain radiography, magnetic resonance imaging, and gross and microscopic evaluation. Preservation of the disc height, annular structure was seen in MSC-transplantation groups compared to the operated control group with no MSC transplantation. Result of the number of remaining transplanted MSCs, the survival rate of NP cells, and apoptosis of NP cells in transplanted discs showed both structural microenvironment and abundant extracellular matrix maintained in 106 MSCs transplanted disc, while less viable cells were detected in 105 MSCs transplanted and more apoptotic cells in 107 MSCs transplanted discs. The results of this study demonstrate that the number of cells transplanted affects the regenerative capability of MSC transplants in experimentally induced degenerating canine discs. It is suggested that maintenance of extracellular matrix by its production from transplanted cells and/or resident cells is important for checking the progression of structural disruption that leads to disc degeneration.
Dorsolateral spinal cord compression at the C2-C3 junction in two Cavalier King Charles spaniels. K. P. Harris, T. C. Saveraid, and S. Rodenas. Vet. Rec. 2011;169(16):416. Quote: Due to the high incidence of Chiari-like malformation (CM) and syringomyelia (SM) in Cavalier King Charles spaniels (CKCS), the presentation of this breed with a history of apparent neck pain often prompts an early suspicion for CM-SM. Conversely, CM-SM findings upon MRI have been reported in many asymptomatic CKCS, and thus other differentials for neck pain such as vertebral trauma, meningioencephalomyelitis or myelocompression must be exhaustively excluded. Cervical spondylomyelopathy (CSM), also referred to as cervical vertebral malformation-malarticulation syndrome, cervical vertebral stenotic myelopathy and wobbler syndrome among other terms, is a common multifactorial neurological disorder affecting mainly large/giant breed dogs. Cases of CSM have been broadly classified by their mechanism of spinal cord and/or nerve root compression as either disc-associated (DA-CSM) or osseous-associated (OA-CSM). This short communication describes dorsolateral compressive lesions of the spinal cord at the C2-C3 junction, similar to those described in giant breed dogs with OA-CSM, in two CKCS with concurrent CM, being evaluated with MRI for neck pain. To the author's knowledge, this is the first report of such MRI findings in this breed. In case 1, a 13.9 kg two-year-old male neutered CKCS presented with a three-month history of intermittent periods of apparent discomfort manifested as very abrupt rising from rest. Two weeks earlier, the owner had observed an isolated episode of ataxia during which the dog fell to the left, had a left-sided head tilt and facial twitching. The dog remained responsive to the owner throughout and returned to normal within 30 minutes. The owner also reported that the dog frequently scratched at one ear (the side unknown). Neurological and otoscopic examination revealed no abnormalities. Moderate to severe hyperaesthesia was evident upon manipulation of the cervical spine. ... It is notable that both dogs were considerably larger than the average CKCS, however, limited conclusions can be drawn from this with such a small number of cases. Identification and histopathological evaluation of further CKCS with dorsolateral myelocompression at C2-C3 and intraspinal cysts is essential to establish the full aetiopathogenesis and clinical effect of these abnormalities.
Intervertebral Disk Herniation. Jonathan M. Levine. NAVC Clinicians Brief. Feb 2012; 18-20. Quote: "Intervertebral disk herniation (IVDH) is abnormal displacement of the nucleus pulposus and/or annulus fibrosus into the vertebral canal or intervertebral foramen. IVDH is the most common cause of spinal cord injury in dogs; some breeds have a lifetime incidence that approaches 20%. ... Myelography, computed tomography (CT), and magnetic resonance imaging (MRI) are typically used to diagnose IVDH.All three imaging modalities can localize spinal cord compression. Many clinicians favor MRI because it is multiplanar and noninvasive, provides data associated with functional outcome, and is the only means of diagnosing certain vertebral column diseases that clinically resemble IVDH (eg, vascular myelopathies)."
Evolution of clinical signs and predictors of outcome after conservative medical treatment for disk-associated cervical spondylomyelopathy in dogs. Steven De Decker, Ingrid M. V. L. Gielen, Luc Duchateau, Anna Oevermann, Ingeborgh Polis, Iris Van Soens, Henri J. J. van Bree,Luc M. L. Van Ham. JAVMA April 2012; 240(7):848-857. Quote: "Objective—To evaluate the evolution of clinical signs and their correlation with results of magnetic resonance imaging (MRI) and transcranial magnetic stimulation (TMS) and to assess potential prognostic variables after conservative medical treatment for disk-associated cervical spondylomyelopathy (DA-CSM) in dogs. Design—Prospective cohort study. Animals—21 client-owned dogs with DA-CSM. Procedures—After neurologic grading, dogs underwent low-field MRI and TMS with measurement of onset latencies and peak-to-peak amplitudes from the extensor carpi radialis and cranial tibial muscles. Dimensions calculated from MRI images were remaining spinal cord area, spinal cord compression ratio, vertebral occupying ratio, vertebral canal height-to-body height ratio, vertebral canal height-to-body length ratio, and vertebral canal compromise ratio. Intraparenchymal signal intensity changes were graded. Dogs were reevaluated 1, 3, 6, 12, and 24 months after initial diagnosis. Results—Outcome was successful in 8 of 21 dogs. Negative outcomes were characterized by rapid progression of clinical signs. All dogs with more severe clinical signs of DA-CSM 1 month after diagnosis had unsuccessful outcomes. Outcome was associated with the remaining spinal cord area and vertebral canal compromise ratio. Prognosis was not associated with severity of clinical signs or results of TMS. There were no significant correlations among clinical signs, MRI findings, and TMS results. Conclusions and Clinical Relevance—Conservative medical treatment of DA-CSM was associated with a guarded prognosis. Selected MRI variables and clinical evolution 1 month after diagnosis can be considered prognostic indicators. The lack of correlation among clinical signs, results of diagnostic imaging, and results of electrophysiologic evaluation in dogs with DA-CSM warrants further investigation."
Incidence of intervertebral disk degeneration–related diseases and associated mortality rates in dogs. Niklas Bergknut, Agneta Egenvall, Ragnvi Hagman, Pia Gustås, Herman A. W. Hazewinkel, Björn P. Meij, Anne-Sofie Lagerstedt. J.Amer.Vet.Med.Assn. June 2012; 2240(11):1300-1309. Quote: "Objective — To determine the incidence and distribution of intervertebral disk (IVD) degeneration–related diseases in a large population of dogs of various breeds, ages, and sexes and to determine mortality rates among dogs with these diseases. ... Because a comprehensive categorization of breeds was not available, the following breeds were classified as chondrodystrophic on the basis of previously published information1,4,7,12,23– 31: Basset Hound, Beagle, Standard Dachshund, Miniature Dachshund, English Bulldog, French Bulldog, American Cocker Spaniel, English Cocker Spaniel, Bichon Frisé, Jack Russell Terrier, Drever, Pug, Miniature Poodle, Cavalier King Charles Spaniel, Shih Tzu, Papillion, and Tibetan Spaniel. ... Design — Epidemiological study. Sample — Insurance data for dogs with veterinary health-care and life insurance coverage (n = 665,249 and 552,120, respectively)[cavalier King Charles spaniels included]. Procedures — Insurance claim records of 1 company in Sweden were searched to identify dogs with IVD degeneration–related diseases; incidence and mortality rates were determined for affected dogs < 12 years old and < 10 years old, respectively. Only the first paid IVD degeneration–related claim for a dog was included in incidence rate calculations. Results — The incidence rate of IVD degeneration–related diseases was 27.8 (95% confidence interval [CI], 27.2 to 28.4) occurrences/10,000 dog-years at risk (DYAR), indicating that approximately 0.3% of dogs/y in this population were affected. Miniature Dachshund was the most highly represented breed, followed by Standard Dachshund and Doberman Pinscher (237.1 [95% CI, 212.9 to 261.4], 141.5 [95% CI, 135.5 to 147.4], and 88.6 [95% CI, 72.1 to 105.2] occurrences/10,000 DYAR, respectively). The incidence rate of IVD degeneration–related disease was greater in male than in female dogs and increased with age. Overall mortality rate attributed to IVD degeneration–related diseases was 9.4 (95% CI, 8.9 to 9.8) deaths/10,000 DYAR and was greater in males than in females. Conclusions and Clinical Relevance — Differences in incidence rates among various breeds suggested a genetic involvement. Knowledge of the distribution of IVD degeneration–related diseases among dogs of various breeds and ages may facilitate early diagnosis and preemptive treatments in patients at risk for developing these diseases."
Intervertebral disc disease in dogs – Part 1: A new histological grading scheme for classification of intervertebral disc degeneration in dogs. N. Bergknut, B.P. Meij, R. Hagman, K.S. de Nies, J.P. Rutges, L.A. Smolders, L.B. Creemers, A.S. Lagerstedt, H.A.W. Hazewinkel, G.C.M. Grinwis. Vet.J. July 2012. Quote: "Intervertebral disc (IVD) degeneration is common in dogs and can lead to serious disorders. Current treatments can relieve clinical signs of disease, but do not restore IVD function. The development of regenerative strategies for IVD dysfunction requires detailed knowledge of the pathogenesis of IVD degeneration and its underlying mechanisms. Histological examination of IVDs at different stages of degeneration might provide this knowledge, but as there is currently no histological grading scheme for canine IVD degeneration, the aim of this study, which is the first of a two-part series, was to design and validate an appropriate scheme. Three independent observers evaluated 35 IVDs at different stages of degeneration using the scheme. Glycosaminoglycan contents of the nucleus pulposus and macroscopic grading according to Thompson, which are considered ‘gold standards’ for IVD degeneration, were used to validate the scheme. Reproducibility was assessed by analysing the inter-observer reliability of all individual variables of the grading scheme, using a weighted κ analysis. Significant correlations were found between Thompson grading and total histological score (r = 0.94; P < 0.01) and between glycosaminoglycan content and total histological score (r = −0.72; P < 0.01). Most individual histological variables showed ‘moderate’ to ‘almost perfect’ inter-observer reliability. The high correlation with the gold standards in combination with the high reproducibility indicates that the proposed histological grading scheme is reliable and objective for classification of IVD degeneration in both chondrodystrophic and non-chondrodystrophic dog breeds."
Intervertebral disc disease in dogs – Part 2: Comparison of clinical, magnetic resonance imaging, and histological findings in 74 surgically treated dogs. Hendrik-Jan C. Kranenburg, Guy C.M. Grinwis, Niklas Bergknut, Ninke Gahrmann, George Voorhout, Herman A.W. Hazewinkel, Björn P. Meij. Vet.J. July 2012. Quote: "The relationship between intervertebral disc (IVD) disease and IVD degeneration remains unclear. The aim of the present study was to compare the clinical severity of IVD herniation (IVDH), determined with a neurological grading system, with findings of magnetic resonance imaging (MRI) and histology using grading systems for IVD degeneration in chondrodystrophic (CD; n = 37) and non-chondrodystrophic (NCD; n = 37) dogs. This study is the second part of a two-part investigation, where the first part involved the development and validation of a histological grading scheme for classification of canine IVD degeneration. IVD degeneration graded on MRI correlated significantly with IVD degeneration graded on histology, but not with pre-operative clinical signs. Hansen type 1 hernias were more common in the cervical and thoracolumbar segments and Hansen type 2 hernias were more common in the lumbosacral segment. Type 1 hernias occurred more often in CD dogs than in NCD dogs, and CD dogs were clinically more severely affected than NCD dogs. The grade of IVD degeneration on MRI was higher in CD dogs than in NCD dogs, but there was no difference between dogs with type 1 and type 2 hernias. No significant differences in histological grade were found between CD and NCD dogs or between type 1 and type 2 hernias. It was possible to conclude that IVD degeneration did not correlate with the neurological severity of IVDH. The extent of degeneration identified on MRI correlated with degeneration seen histologically. Although the MRI grading system reflected the severity of IVD degenerative changes as confirmed by histopathology, it appeared less useful in predicting the clinical implications."
Assessment of the effects of adjunctive gabapentin on postoperative pain after intervertebral disc surgery in dogs. Sonja A. Aghighi, Andrea Tipold, Marion Piechotta, Piotr Lewczuk, Sabine B.R. Kästne. Veterinary Anaesthesia and Analgesia. Nov. 2012; 39(6):636–646. Quote: "Objective: To assess the effect of adjunctive gabapentin (GBP) on pain after thoracolumbar intervertebral disc surgery in dogs. Study design Prospective, randomized, controlled, clinical, ‘blinded’ trial. Animals: Sixty-three client owned dogs undergoing hemilaminectomy. Methods: Dogs were assigned to two treatment groups. The GBP group received gabapentin 10 mg kg−1 orally every 12 hours starting before anaesthesia; the placebo (P) group received empty gelatin capsules. Background analgesia was initiated with intravenous levomethadone 0.6 mg kg−1 (as the combination ‘L-Polamivet) at anaesthesia induction, followed by a fentanyl patch and levomethadone 0.2 mg kg−1 subcutaneously every 8 hours for 24 hours. Pain was assessed by the short form of the Glasgow Composite Measure Pain Score (CMPS-SF) without the gait category, and by a Visual Analogue Scale (VAS). Serum GBP concentrations and cortisol concentrations were measured. Statistical analyses utilized chi square test, Kolmogorov-Smirnov test, two-way analysis of variances for repeated measurements, Wilcoxon test and Friedmann test as relevant. Correlations were tested by Spearman’s and Pearson’s correlation coefficient. p < 0.05 was considered significant. Results: Median CMPS-SF was lower in group GBP than in group P on days 0.5, 1, 4 and 5. However, CMPS-SF and VAS were not significantly different between groups. Both pain scores decreased significantly over time. Cortisol concentrations were not significantly different between groups. Minimum serum concentrations of GBP fell below the detection limit of 1 μg mL−1 in 6 of 29 and 7 of 28 dogs at 24 and 72 hours, respectively. Conclusions and clinical relevance: 10 mg kg−1 GBP orally twice a day did not result in a detectable reduction in pain behaviour compared to background opioid analgesia alone, although a trend to lower pain levels (p < 0.1) was present. Further studies are needed to determine if this is related to effective background analgesia or an ineffective dose of GBP."
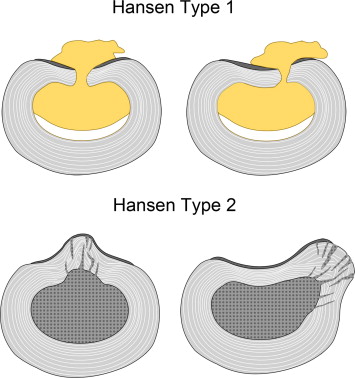 Intervertebral
disc degeneration in the dog. Part 2: Chondrodystrophic and
non-chondrodystrophic breeds. Lucas A. Smolders, Niklas Bergknut, Guy C.M.
Grinwis, Ragnvi Hagman, Anne-Sofie Lagerstedt, Herman A.W. Hazewinkel, Marianna
A. Tryfonidou, Björn P. Meij. Vety.J. March 2013;195(3):292-299. Quote: Dogs can
be grouped into two distinct types of breed based on the predisposition to
chondrodystrophy, namely, non-chondrodystrophic (NCD) and chondrodystrophic
(CD). ... IVD degeneration is more common in CD breeds, which are characterized
by a disturbed endochondral ossification, primarily of the long bones, such that
CD dogs have disproportionally short limbs. Popular CD breeds include, among
others, the (miniature) Dachshund, Basset Hound, French and English Bulldog, Shi
Tzu, miniature Schnauzer, Pekingese, Beagle, Lhasa Apso, Bichon Frisé, Tibetan
Spaniel, Cavalier King Charles Spaniel, Welsh Corgi, and the
American Cocker Spaniel. ... In addition to a different process of
endochondral ossification, NCD and CD breeds have different characteristics of
intravertebral disc (IVD) degeneration and IVD degenerative diseases. The
anatomy, physiology, histopathology, and biochemical and biomechanical
characteristics of the healthy and degenerated IVD are discussed in the first
part of this two-part review. This second part describes the similarities and
differences in the histopathological and biochemical characteristics of IVD
degeneration in CD and NCD canine breeds and discusses relevant aetiological
factors of IVD degeneration.
Intervertebral
disc degeneration in the dog. Part 2: Chondrodystrophic and
non-chondrodystrophic breeds. Lucas A. Smolders, Niklas Bergknut, Guy C.M.
Grinwis, Ragnvi Hagman, Anne-Sofie Lagerstedt, Herman A.W. Hazewinkel, Marianna
A. Tryfonidou, Björn P. Meij. Vety.J. March 2013;195(3):292-299. Quote: Dogs can
be grouped into two distinct types of breed based on the predisposition to
chondrodystrophy, namely, non-chondrodystrophic (NCD) and chondrodystrophic
(CD). ... IVD degeneration is more common in CD breeds, which are characterized
by a disturbed endochondral ossification, primarily of the long bones, such that
CD dogs have disproportionally short limbs. Popular CD breeds include, among
others, the (miniature) Dachshund, Basset Hound, French and English Bulldog, Shi
Tzu, miniature Schnauzer, Pekingese, Beagle, Lhasa Apso, Bichon Frisé, Tibetan
Spaniel, Cavalier King Charles Spaniel, Welsh Corgi, and the
American Cocker Spaniel. ... In addition to a different process of
endochondral ossification, NCD and CD breeds have different characteristics of
intravertebral disc (IVD) degeneration and IVD degenerative diseases. The
anatomy, physiology, histopathology, and biochemical and biomechanical
characteristics of the healthy and degenerated IVD are discussed in the first
part of this two-part review. This second part describes the similarities and
differences in the histopathological and biochemical characteristics of IVD
degeneration in CD and NCD canine breeds and discusses relevant aetiological
factors of IVD degeneration.
Intervertebral Disk Degeneration in Dogs: Consequences, Diagnosis, Treatment, and Future Directions. N.D. Jeffery, J.M. Levine, N.J. Olby and V.M. Stein. J.Vet.Int.Med. Nov. 2013;27(6):1318–1333. Quote: "Evidence of intervertebral disk degeneration (IVDD) is extremely common in dogs, and its prevalence increases with age. It has many important consequences because degeneration of the intervertebral disks often is a prelude to disk herniation, which can injure the spinal cord, spinal nerves, or both. This review summarizes the advances in diagnosis and treatment of IVDD that have been made since the 1950s when the first detailed description of the degenerative changes was published. It also discusses new approaches to treatment of the associated spinal cord injury and new methods by which to classify injury severity that are currently under development."
Influence of duration of clinical signs on surgical treatment results of 16 dogs with intervertebral disc disease (IVDD). Marcin Wrzosek, Zdzisław Kiełbowicz, Elżbieta Giza, Marta Płonek, Józef Nicpoń. Bull Vet Inst Pulawy. 2014:58:277-281. Quote: "The purpose of this study was to evaluate the outcome of surgical treatment in 16 dogs, depending on the animal’s age, body weight, deep pain perception, and time from the onset of neurological symptoms to the consultation with a veterinary neurologist and successive surgery. Sixteen dogs diagnosed with cervical (n = 11) [including a cavalier King Charles spaniel] or thoracolumbar (n = 5) disc extrusions underwent spinal surgeries (eleven ventral slots and five hemilaminectomies). The success rate of surgical treatment was 64.3% in dogs with preserved nociception. No association between the animal’s age or body weight and the result of surgical treatment was found. A successful surgical outcome was more likely when the symptom-to-surgery time was shorter."
Medical Infrared Imaging (Thermography) of Type I Thoracolumbar Disk
Disease in Chondrodystrophic Dogs. Brian P.
 Grossbard, Catherine A.
Loughin, Dominic J. Marino, Leonard J. Marino, Joseph Sackman, Scott E.
Umbaugh, Patrick S. Solt, Jakia Afruz, Peter Leando, Martin L. Lesser,
Meredith Akerman. Vet. Surgery. Oct. 2014;43(7):869-876. Quote: "Objective:
to: (1) determine the success of medical infrared imaging (MII) in
identifying dogs with TLIVDD, (2) compare MII localization with magnetic
resonance imaging (MRI) results and surgical findings, and (3) determine if
the MII pattern returns to that of normal dogs 10 weeks after decompression
surgery. Study Design: Prospective case series. Animals: Chondrodystrophic
dogs (n=58) with Type I TLIVDD and 14 chondrodystrophic dogs with no
evidence of TLIVDD. Methods: Complete neurologic examination, MII, and MRI
studies were performed on all dogs. Dogs with type I TLIVDD had
decompressive surgery and follow-up MII was performed at 10 weeks. Pattern
analysis software was used to differentiate between clinical and control
dogs, and statistical analysis using anatomic regions of interest on the
dorsal views were used to determine lesion location. Recheck MII results
were compared with control and pre-surgical images. Results: Computer
recognition pattern analysis was 90% successful in differentiating normal
dogs from dogs affected by TLIVDD and 97% successful in identifying the
abnormal intervertebral disc space in dogs with TLIVDD. Statistical
comparisons of the ROI mean temperature were unable to determine the
location of the disc herniation. Recheck MII patterns did not normalize and
more closely resembled the clinical group. Conclusions: MII was 90%
successful differentiating between normal dogs and 97% successful in
identifying the abnormal intervertebral disc space in dogs with TLIVDD.
Abnormal intervertebral disc space localization using ROI mean temperature
analysis was not successful. MII patterns 10 weeks after surgery do not
normalize."
Grossbard, Catherine A.
Loughin, Dominic J. Marino, Leonard J. Marino, Joseph Sackman, Scott E.
Umbaugh, Patrick S. Solt, Jakia Afruz, Peter Leando, Martin L. Lesser,
Meredith Akerman. Vet. Surgery. Oct. 2014;43(7):869-876. Quote: "Objective:
to: (1) determine the success of medical infrared imaging (MII) in
identifying dogs with TLIVDD, (2) compare MII localization with magnetic
resonance imaging (MRI) results and surgical findings, and (3) determine if
the MII pattern returns to that of normal dogs 10 weeks after decompression
surgery. Study Design: Prospective case series. Animals: Chondrodystrophic
dogs (n=58) with Type I TLIVDD and 14 chondrodystrophic dogs with no
evidence of TLIVDD. Methods: Complete neurologic examination, MII, and MRI
studies were performed on all dogs. Dogs with type I TLIVDD had
decompressive surgery and follow-up MII was performed at 10 weeks. Pattern
analysis software was used to differentiate between clinical and control
dogs, and statistical analysis using anatomic regions of interest on the
dorsal views were used to determine lesion location. Recheck MII results
were compared with control and pre-surgical images. Results: Computer
recognition pattern analysis was 90% successful in differentiating normal
dogs from dogs affected by TLIVDD and 97% successful in identifying the
abnormal intervertebral disc space in dogs with TLIVDD. Statistical
comparisons of the ROI mean temperature were unable to determine the
location of the disc herniation. Recheck MII patterns did not normalize and
more closely resembled the clinical group. Conclusions: MII was 90%
successful differentiating between normal dogs and 97% successful in
identifying the abnormal intervertebral disc space in dogs with TLIVDD.
Abnormal intervertebral disc space localization using ROI mean temperature
analysis was not successful. MII patterns 10 weeks after surgery do not
normalize."
Disc Prostheses: Cervical Disc Arthroplasty. Filippo Adamo. ACVS. October 2014.
Modulation of the proteoglycan receptor PTPσ promotes recovery after spinal cord injury. Bradley T. Lang, Jared M. Cregg, Marc A. DePaul, Amanda P. Tran, Kui Xu, Scott M. Dyck, Kathryn M. Madalena, Benjamin P. Brown, Yi-Lan Weng, Shuxin Li, Soheila Karimi-Abdolrezaee, Sarah A. Busch, Yingjie Shen, Jerry Silver. Nature. December 2014. Quote: "Contusive spinal cord injury leads to a variety of disabilities owing to limited neuronal regeneration and functional plasticity. It is well established that an upregulation of glial-derived chondroitin sulphate proteoglycans (CSPGs) within the glial scar and perineuronal net creates a barrier to axonal regrowth and sprouting. Protein tyrosine phosphatase σ (PTPσ), along with its sister phosphatase leukocyte common antigen-related (LAR) and the nogo receptors 1 and 3 (NgR), have recently been identified as receptors for the inhibitory glycosylated side chains of CSPGs. Here we find in rats that PTPσ has a critical role in converting growth cones into a dystrophic state by tightly stabilizing them within CSPG-rich substrates. We generated a membrane-permeable peptide mimetic of the PTPσ wedge domain that binds to PTPσ and relieves CSPG-mediated inhibition. Systemic delivery of this peptide over weeks restored substantial serotonergic innervation to the spinal cord below the level of injury and facilitated functional recovery of both locomotor and urinary systems. Our results add a new layer of understanding to the critical role of PTPσ in mediating the growth-inhibited state of neurons due to CSPGs within the injured adult spinal cord."
Potassium Channel Antagonists 4-Aminopyridine and the T-Butyl Carbamate Derivative of 4-Aminopyridine Improve Hind Limb Function in Chronically Non-Ambulatory Dogs; A Blinded, Placebo-Controlled Trial. Ji-Hey Lim, Audrey C. Muguet-Chanoit, Daniel T. Smith, Eric Laber, Natasha J. Olby. PLOS One. December 2014. Quote: "4-Aminopyridine (4-AP) blocks voltage gated potassium channels, restoring conduction to demyelinated axons and improving function in demyelinating conditions, but its use is associated with adverse effects and benefit in spinal cord injury is limited. Derivatives of 4-AP have been developed to improve clinical efficacy while reducing toxicity. We compared the therapeutic effects of orally administered 4-AP and its t-butyl carbamate derivative (t-butyl) with placebo in dogs that had suffered an acute spinal cord injury that left them chronically paralyzed. Nineteen dogs were entered into the trial, conducted in two-week treatment blocks starting with placebo, followed by random assignment to 4-AP or t-butyl, a washout and then the opposite medication followed by placebo. Investigators and owners were blinded to treatment group. Primary outcome measures included open field gait score (OFS), and treadmill based stepping score and regularity index, with additional secondary measures also considered. Thirteen of 19 dogs completed the protocol. Two were euthanized due to unrelated heath problems, two developed side effects and two were unable to complete for unrelated reasons. Dogs showed significant improvement in supported stepping score (from 17.39 to 37.24% with 4-AP; 16.85 to 29.18% with t-butyl p<0.0001) and OFS (from 3.63 to 4.73 with 4-AP; 3.78 to 4.45 with t-butyl, p = 0.005). Response was individually variable and most dramatic in three dogs that were able to walk without support with treatment. No significant difference was found between 4-AP and t-butyl. No adverse effects were reported with t-butyl but gastrointestinal upset and seizures were observed in two dogs with 4-AP. In conclusion, both 4-AP and t-butyl significantly improved supported stepping ability in dogs with chronic spinal cord injury with no adverse effects noted with t-butyl. Drug response varied widely between individuals, highlighting the need to understand the factors that influence canine and human patients' response to therapy."
Will There be a Role for Disc Prostheses in Small Animals? Filippo Adamo and Franck Forterre. In, Advances in Intervertebral Disc Disease in Dogs and Cats, First Edition. Edited by James M. Fingeroth and William B. Thomas. John Wiley & Sons, Inc. February 2015.
Canine chondrodystrophic intervertebral disc disease (Hansen type I disc disease). Clare Rusbridge. BMC Musculoskeletal Disorders. December 2015; 16(Suppl 1):S11. Quote: "Intervertebral disc disease (IVDD) is the most common spinal disease in dogs. Chondrodystrophic dogs, which have disproportionably short and curved limbs, are predisposed to Hansen type I IVDD and of these the miniature Dachshund is over represented, is more likely to be presented at an earlier age and is at greater risk of a severe spinal cord injury. The tendency for IVDD in Dachshunds is inherited and a major locus on chromosome 12 harbours genetic variations affecting the development of intervertebral disc calcification. Hansen type I disc degeneration is thought to occur because of loss of notochordal cells which produce proteoglycans which “hold water” in the disc. Chondrodystrophic dogs have a primary deficiency of notochordal cells, a study found that large notochordal cells in the nucleus pulposus of chondrodystrophoid dogs formed 13% of the cell population in young dogs and fell to 0.4% in adults, whereas they were the predominant cell type in the nonchondrodystrophoid dogs at all ages. Thus chondrodystrophoid dogs suffer early degenerative changes in the disc and a concomitant reduction in proteoglycan content, increased collagen, and loss of water content making the discs likely to herniate. Certain lifestyle factors may increase or decrease risk of IVDD and this is currently under investigation. There is a suggestion that exercise (including stair climbing) reduces the incidence of disc calcification. By contrast it has been hypothesized that obesity/lack of postural muscle strength may increase risk. Dachshunds with intervertebral disc extrusion had significantly smaller cross sectional area and greater fat infiltration in the epaxial muscles (muscles which lie dorsal to the horizontal septum of the vertebrae which mobilize and globally stabilize the trunk) compared to dogs presenting with fibrocartilagenous embolism (another acute onset intervertebral disc related spinal disease). In addition chondrodystrophic dogs may have increased risk of IVVD if they have a more extreme conformation e.g. Dachshunds that have a longer back and shorter limbs are more at risk and breeds with a comparatively heavy head such as the Bassett Hound may be more at risk of cervical disc disease. Breeds with a tendency for kyphoscoliosis such as the French Bulldog may be more at risk of IVDD in the IVDs adjacent to a vertebral malformation. This presentation details the pathogeneis, clinical presentation, diagnosis and treatment of IVDD in chondrodystrophic dogs."
Determination of the Accuracy of Neurological Data, Survey Radiography, Computed Tomography (CT), Myelography and CT Myelography for Detection of the Seat of Intervertebral Disc Herniation in Dogs. Mohammed Abdel-Hakiem, Masaaki Katayama, Ahmed Saleh, Haroun Youssef, Yasuhiko Okamura, Yuji Uzuka. J. Advanced Vet. Research. January 2016;6(1):44-52. Quote: "The present study was carried out to determine the accuracy of different tools for detection of the seat of intervertebral disc (IVD) herniation in dogs. Forty-six dogs of different breeds were included in this study. [46 miniature Dachshunds, 5 Chhihuahuas, 3 toy poodles, 3 Yorkshire terriers, and 2 cavalier King Charles spaniels, among others]. The neurological examination and plain radiography were performed for all dogs. Computed tomography (CT), myelography and CT myelography were performed for 38, 33 and 31 dogs respectively. The results showed that the Miniature Dachshund is the most common breed suffering IVDD (39.13%), ... then the Cavalier King Charles Spaniel (12.5%) [with a combined total of 11 lesions]. ... C2-3 was the most affected site in the cervical region (13.37%), while L2-3 is considered the highly affected thoracolumbar site (11.4%) followed by T13-L1 and L1-2 (10.23% for each). The accuracy of neurological examination, plain radiography, CT, myelography and CT myelography for determining the site of the lesion was calculated as 54.3, 30.4, 65.8, 84.85 and 100%, respectively. Moreover, the accuracy of CT, myelography and CT myelography for detection of the side of the lesion was 44.74, 54.54 and 93.9% respectively. ... The results of this study suggested that the neurological examination and survey radiography are not reliable for detection of the site of IVD herniation. The accuracy of the CT increases in the chondrodystrophic breeds, which have chronic lesions due to the mineralization of the extruded disc materials. The myelography is considered a valuable tool in the detection of the lesion, especially in the smaller sized dogs. The CT myelography is considered the bset tool in this study for determining the site of IVD herniation and its laterality in dogs."
Clinical characterization of thoracolumbar and lumbar intervertebral disk extrusions in English Cocker Spaniels. Thomas J.A. Cardy, Caitlin E. Tzounos, Holger A. Volk, Steven De Decker. JAVMA. February 2016;248(4):405-412. Quote: Oojective: To assess the anatomic distribution of thoracolumbar and lumbar intervertebral disk extrusions (IVDEs) in English Cocker Spaniels as compared with findings in Dachshunds and to characterize clinical findings in English Cocker Spaniels with thoracolumbar or lumbar IVDEs affecting various regions of the vertebral column. Design: Retrospective observational study. Animals: 81 English Cocker Spaniels and 81 Dachshunds with IVDEs. Procedures: Signalment, clinical signs, neurologic examination findings, and affected intervertebral disk spaces (IVDSs) were recorded for both breeds. Management methods and outcomes were recorded for English Cocker Spaniels. Lesions were categorized as thoracolumbar (IVDSs T9–10 through L1–2), midlumbar (L2–3 through L4–5), or caudal lumbar (L5–6 through L7–S1). Results: Midlumbar and caudal lumbar IVDEs were significantly more common in English Cocker Spaniels than in Dachshunds. English Cocker Spaniels with caudal lumbar IVDEs had a longer median duration of clinical signs before evaluation and more commonly had unilateral pelvic limb lameness or spinal hyperesthesia as the predominant clinical sign than did those with IVDEs at other sites. Those with caudal lumbar IVDEs less commonly had neurologic deficits and had a higher median neurologic grade (indicating lesser severity), shorter mean postoperative hospitalization time, and faster mean time to ambulation after surgery than those with other sites affected. These variables did not differ between English Cocker Spaniels with thoracolumbar and midlumbar IVDEs. Conclusions and Clinical Relevance: Caudal and midlumbar IVDEs were more common in English Cocker Spaniels than in Dachshunds. English Cocker Spaniels with caudal lumbar IVDE had clinical signs and posttreatment responses that differed from those in dogs with midlumbar or thoracolumbar IVDE.
Recognition and Breed Specificity of Canine Spondyloarthropathy. Bruce M. Rothschild, Sabine M. Breit. J. Spine. March 2016;5(2):293. Quote: Human diseases sometimes represented across phylogenetic lines. Their recognition is at times compromised by differential (between human and veterinary medicine) use of diagnostic terms. A major impetus to such change is recognition of additional treatment options that would not be considered for the replaced diagnosis/ category. Canine syndesmophytes are recognized as identifier for spondyloarthropathy. This study examines the breed-specificity of those changes. The axial skeletons and peripheral joints (when available) of 1323 dogs, identified to breed [including 26 cavalier King Charles spaniels], were examined for evidence of syndesmophytes and sacroiliac joint disease. Syndesmophytes were found in 315 of 1323 axial skeletons examined, extremely common in Boxer and German Shephard; rare, in Beagle, Chihauahua, Dachshund, Maltese and Pug. First noted at 2 years of age, its prevalence increased geometrically over the next 13 years. All affected individuals weighed more than 2 kilograms and prevalence increased geometrically through 39.9 kilograms. Spondyloarthropathy was present in 17.3% of brachycephalic, contrasted with 35.0% of mesticephalic dogs [Chi square = 16.972, p < 0.0001]. Presence of syndesmophytes identified the underlying arthritis as spondyloarthropathy, not osteoarthritis. Recognition of the vertebral findings as characteristic of this inflammatory arthritis affords an opportunity for controlling the disease process and improving quality of life of the afflicted dog.
Differential diagnosis of vertebral spinous process deviations in archaeological and modern domestic dogs. Dennis F. Lawler, Chris Widga, David A. Rubin, Jennifer A. Reetz, Richard H. Evans, Basil P. Tangredi, Richard M. Thomas, Terrence J. Martin, Charles Hildebolt, Kirk Smith, Daniel Leib, Jill E. Sackman, James G. Avery, Gail K. Smith. J. Archaeological Science: Reports. July 2016. Quote: Paleopathological study of domestic animal remains can elucidate human-domesticate relationships, when all reasonable differential diagnoses are considered. Deviated spinous processes found on ancient domesticated dog vertebrae have been assumed to result from pack burdens, although consideration of diagnostic alternatives has been unclear. To more thoroughly assess the potential significance of these features, we first generated an extensive differential diagnosis of potential causes. Broad causal categories included: (i) morphological; (ii) infectious; (iii) taphonomic; (iv) life history (in utero to death), with numerous subcategories that sometimes overlap. We then evaluated these possibilities through an observational and radiology study of 15 ancient deliberate domestic dog burials (191 vertebrae) from the midwestern USA, dating between 10,130 and 200 years ago. Archaeological specimens from the UK were included to evaluate for geographic uniqueness of our observations. We characterized deviations of spinous processes of cervical (n = 74), thoracic (n = 51), lumbar (n = 60), and sacral (n = 6) vertebrae. Affected spinous processes were found in 34% of cervical vertebrae, 63% of thoracic vertebrae, 78% of lumbar vertebrae, and 50% of sacral vertebrae. Four types of spinous process deviations were observed: (a) lateral leaning from the base but not otherwise deviated; (b) lateral curving at some point above the base; (c) bowing because of multiple curves; and (d) torsion along the vertical axis. Computed tomography and micro-computed tomography were essential tools for establishing differential diagnoses. Highlights: Deviated vertebral spinous processes in dogs have been attributed historically to use as pack animals. A differential diagnosis for deviated spinous processes in domesticated dogs is presented. Observational and imaging studies indicate that deviated vertebral spinous processes have complex origins. Computed tomography and micro-computed tomography were essential tools for establishing differential diagnoses.
Prevalence of spinous process impingement in thoracic vertebrae on radiographs of clinically-unaffected dogs. F. Thierry, K. Bradley, C. Warren-Smith. J. Small Anim. Pract. October 2016. Quote: Objectives: To assess the prevalence of impinged spinous processes in asymptomatic dogs. Methods: One hundred and ninety lateral thoracic radiographs of asymptomatic dogs [including cavalier King Charles spaniels] radiographed for reasons other than spinal pain, were retrospectively reviewed by two board-certified radiologists. Images were assessed for impinged spinous processes and graded for narrowing, sclerosis or remodelling of the spinous processes. Results: The prevalence of impinged spinous processes in unaffected dogs was 33·2%. Seventy-five of 79 (95%) lesions were located between T8 and T11. Impingement of the spinous processes was more common in older dogs and larger dogs displayed more frequent and more severe impingement of the spinous processes compared with smaller breeds. Clinical Significance: Spinous process impingement is common in animals with no history of spinal pain, indicating that this radiographic finding should be interpreted with caution.
Recurrence of disk herniation following percutaneous laser disk ablation in dogs with a history of thoracolumbar intervertebral disk herniation: 303 cases (1994–2011). Danielle R. Dugat, Kenneth E. Bartels, Mark E. Payton. J.A.V.M.A. December 2016; doi: 10.2460/javma.249.12.1393. Quote: Objectdive: To determine rate of recurrence of disk herniation in dogs that underwent percutaneous laser disk ablation (PLDA) because of a previous episode of suspected or confirmed thoracolumbar intervertebral disk herniation (IVDH). Design: Retrospective case series. Animals: 303 dogs that underwent PLDA and for which a minimum of 3 years of follow-up information was available (n = 294) or for which recurrence was documented within 3 years after the procedure [including one cavalier King Charles spaniel]. Procedures: Information on signalment, previous episodes of IVDH, specifics of the PLDA procedure, and recurrence was obtained from the medical records. Owners were contacted to complete a questionnaire regarding outcome and recurrence. Results: 60 of the 303 (19.8%) dogs had an episode of suspected or confirmed IVDH after undergoing PLDA, but only 11 of the 303 (3.6%) dogs had a recurrence of IVDH confirmed by means of CT or MRI and hemilaminectomy. Recurrence rate following PLDA was not significantly different between dogs that had been treated medically for previous episodes of IVDH and dogs that had been treated surgically. Overall, 270 of 286 (94.4%) owners reported that their dog was the same (109 [38.1%]) or improved (161 [56.3%]) immediately after PLDA, and 265 (92.7%) owners rated their satisfaction with the procedure as ≥ 9 on a scale from 1 (completely dissatisfied) to 10 (completely satisfied). Conclusion and Clinical Relevance: Results suggested that PLDA was a relatively safe, minimally invasive procedure associated with a low rate of recurrence of disk herniation when performed in dogs with a history of previous episodes of suspected or confirmed IVDH.
Proportion recovery and times to ambulation for non-ambulatory dogs with thoracolumbar disc extrusions treated with hemilaminectomy or conservative treatment: A systematic review and meta-analysis of case-series studies. L. Langerhuusa, J. Milesb. Vet. J. February 2017;220:7-16. Quote: Thoracolumbar intervertebral disc extrusion is a common cause of spinal cord dysfunction in dogs. Peer-reviewed studies reporting treatment of predominantly chondrodystrophic dogs with disc extrusion with loss of ambulation with either hemilaminectomy or conservative treatment (rest, analgesics and anti-inflammatories) were evaluated in a systematic review of the literature. Generally, the level of evidence available was low with no controlled studies and only case series available. In the meta-analysis, there was a clear trend to a greater proportion of dogs recovering and returning faster to ambulation for dogs treated with hemilaminectomy than for conservatively treated dogs. The mean proportions that recovered for neurological grades 3, 4 and 5 were 93, 93 and 61% for those treated with hemilaminectomy, and 79, 62 and 10% for those treated conservatively (Grade 3 – non-ambulatory paraparetic dogs; grade 4 – paraplegic dogs with intact deep pain perception; grade 5 – paraplegic dogs without intact deep pain perception). Due to the use of case series, these results represent between-study comparisons, thereby increasing the risk of selection bias and other biases. Data presented in this review support the current recommendations for surgical management of non-ambulatory dogs with disc-extrusion, but controlled clinical studies comparing outcomes are necessary to confirm these findings.
Evaluation of T2-weighted versus short-tau inversion recovery sagittal sequences in the identification and localization of canine intervertebral disc extrusion with low-field magnetic resonance imaging. Daniel Housley, Abby Caine, Giunio Cherubini, Olivier Taeymans. Vet. Rad. & Ultra. April 2017. Quote: Sagittal T2-weighted sequences (T2-SAG) are the foundation of spinal protocols when screening for the presence of intervertebral disc extrusion. We often utilize sagittal short-tau inversion recovery sequences (STIR-SAG) as an adjunctive screening series, and experience suggests that this combined approach provides superior detection rates. We hypothesized that STIR-SAG would provide higher sensitivity than T2-SAG in the identification and localization of intervertebral disc extrusion. We further hypothesized that the parallel evaluation of paired T2-SAG and STIR-SAG series would provide a higher sensitivity than could be achieved with either independent sagittal series when viewed in isolation. This retrospective diagnostic accuracy study blindly reviewed T2-SAG and STIR-SAG sequences from dogs (n = 110) with surgically confirmed intervertebral disc extrusion [including 6 cavalier King Charles spaniels]. A consensus between two radiologists found no significant difference in sensitivity between T2-SAG and STIR-SAG during the identification of intervertebral disc extrusion (T2-SAG: 92.7%, STIR-SAG: 94.5%, P = 0.752). Nevertheless, STIR-SAG accurately identified intervertebral disc extrusion in 66.7% of cases where the evaluation of T2-SAG in isolation had provided a false negative diagnosis. Additionally, one radiologist found that the parallel evaluation of paired T2-SAG and STIR-SAG series provided a significantly higher sensitivity than T2-SAG in isolation, during the identification of intervertebral disc extrusion (T2-SAG: 78.2%, paired T2-SAG, and STIR-SAG: 90.9%, P = 0.017). A similar nonsignificant trend was observed when the consensus of both radiologists was taken into consideration (T2-SAG: 92.7%, paired T2-SAG, and STIR-SAG = 97.3%, P = 0.392). We therefore conclude that STIR-SAG is capable of identifying intervertebral disc extrusion that is inconspicuous in T2-SAG, and that STIR-SAG should be considered a useful adjunctive sequence during preliminary sagittal screening for intervertebral disc extrusion in low-field magnetic resonance.
FGF4 retrogene on CFA12 is responsible for chondrodystrophy and intervertebral disc disease in dogs. Emily A. Brown, Peter J. Dickinson, Tamer Mansour, Beverly K. Sturges, Miriam Aguilar, Amy E. Young, Courtney Korff, Jenna Linda, Cassandra L. Ettinger, Samuel Varon, Rachel Pollard, C. Titus Brown, Terje Raudsepp, Danika L. Bannasch. PNAS. October 2017; doi: 10.1073/pnas.17090821. Quote: Chondrodystrophy in dogs is defined by dysplastic, shortened long bones and premature degeneration and calcification of intervertebral discs. Independent genome-wide association analyses for skeletal dysplasia (short limbs) within a single breed (PBonferroni = 0.01) and intervertebral disc disease (IVDD) across breeds (PBonferroni = 4.0 × 10−10) both identified a significant association to the same region on CFA12. Whole genome sequencing identified a highly expressed FGF4 retrogene within this shared region. The FGF4 retrogene segregated with limb length and had an odds ratio of 51.23 (95% CI = 46.69, 56.20) for IVDD. Long bone length in dogs is a unique example of multiple disease-causing retrocopies of the same parental gene in a mammalian species. FGF signaling abnormalities have been associated with skeletal dysplasia in humans, and our findings present opportunities for both selective elimination of a medically and financially devastating disease in dogs and further understanding of the ever-growing complexity of retrogene biology.
The Effect of Electromagnetic Fields on Post-Operative Pain and Locomotor
Recovery in Dogs with Acute, Severe Thoracolumbar Intervertebral Disc
Extrusion: A Randomized Placebo-Controlled, Prospective Clinical Trial.
 Natalia Zidan, Joe Fenn, Emily Griffith, Peter J. Early, Chris L. Mariani,
Karen R. Muñana, Julien Guevar, Natasha J. Olby. J. Neurotrauma. August
2018;35:1726-1736. Quote: Spinal cord injury (SCI) attributed to acute
intervertebral disc extrusions (IVDEs) is common in dogs and is treated by
surgical decompression. Dogs with sensorimotor complete injuries have an
incomplete recovery. Pulsed electromagnetic fields (PEMFs) reduce
post-operative pain through anti-inflammatory effects and there is growing
evidence for neuroprotective effects. This randomized, controlled clinical
trial evaluated the effect of PEMF on post-operative pain and neurological
recovery in dogs with surgically treated sensorimotor complete SCI
attributed to acute IVDE. Sixteen dogs with surgically treated complete
thoracolumbar SCI were randomized to receive PEMF (15 min every 2 h for 2
weeks then twice-daily for 4 weeks) or placebo starting immediately after
diagnosis. The primary outcome was gait score at 2 weeks. Secondary measures
of gait, pain perception, and proprioceptive function were evaluated at 2
and 6 weeks. Plasma glial fibrillary acidic protein (GFAP) concentration was
measured as an SCI biomarker. Post-operative pain was quantified by
measuring mechanical sensory thresholds (MSTs) at control and surgical
sites. There was no significant difference in demographics or GFAP
concentration between the two groups at trial entry. There was no difference
in primary outcome or in secondary measures of gait, but proprioceptive
placing was significantly better at 6 weeks and GFAP concentrations were
significantly lower at 2 weeks in the PEMF group. MSTs were significantly
higher in the PEMF-treated group. We conclude that PEMF reduced
incision-associated pain in dogs post-surgery for IVDE and may reduce extent
of SCI and enhance proprioceptive placing. Larger clinical trials are
warranted.
Natalia Zidan, Joe Fenn, Emily Griffith, Peter J. Early, Chris L. Mariani,
Karen R. Muñana, Julien Guevar, Natasha J. Olby. J. Neurotrauma. August
2018;35:1726-1736. Quote: Spinal cord injury (SCI) attributed to acute
intervertebral disc extrusions (IVDEs) is common in dogs and is treated by
surgical decompression. Dogs with sensorimotor complete injuries have an
incomplete recovery. Pulsed electromagnetic fields (PEMFs) reduce
post-operative pain through anti-inflammatory effects and there is growing
evidence for neuroprotective effects. This randomized, controlled clinical
trial evaluated the effect of PEMF on post-operative pain and neurological
recovery in dogs with surgically treated sensorimotor complete SCI
attributed to acute IVDE. Sixteen dogs with surgically treated complete
thoracolumbar SCI were randomized to receive PEMF (15 min every 2 h for 2
weeks then twice-daily for 4 weeks) or placebo starting immediately after
diagnosis. The primary outcome was gait score at 2 weeks. Secondary measures
of gait, pain perception, and proprioceptive function were evaluated at 2
and 6 weeks. Plasma glial fibrillary acidic protein (GFAP) concentration was
measured as an SCI biomarker. Post-operative pain was quantified by
measuring mechanical sensory thresholds (MSTs) at control and surgical
sites. There was no significant difference in demographics or GFAP
concentration between the two groups at trial entry. There was no difference
in primary outcome or in secondary measures of gait, but proprioceptive
placing was significantly better at 6 weeks and GFAP concentrations were
significantly lower at 2 weeks in the PEMF group. MSTs were significantly
higher in the PEMF-treated group. We conclude that PEMF reduced
incision-associated pain in dogs post-surgery for IVDE and may reduce extent
of SCI and enhance proprioceptive placing. Larger clinical trials are
warranted.
Effect of Targeted Pulsed Electromagnetic Field Therapy on Canine Postoperative Hemilaminectomy: A Double-Blind, Randomized, Placebo-Controlled Clinical Trial. Leilani X. Alvarez, John McCue, Nathaniel K. Lam, Gulce Askin, Philip R. Fox. J. Amer. Anim. Hosp. Assn. March 2019;55(2):83-91. Quote: Intervertebral disc disease is one of the leading causes of paralysis in dogs. Pulsed electromagnetic field (PEMF) therapy has been advocated for improving wound healing and pain reduction; however, robust clinical trials are lacking. The present prospective, double-blind, placebo-controlled trial evaluated targeted PEMF therapy administered to 53 client-owned dogs who underwent hemilaminectomy for naturally occurring disk extrusion intervertebral disc disease. The dogs were randomized to receive either targeted PEMF (n = 27) or placebo treatment (n = 28). Wound healing, evaluated by visual analog score and wound evaluation scale, was significantly improved at 6 wk postoperatively in the treatment compared with the control group (P = .010 and .023, respectively). Pain medications were administered less frequently in dogs receiving PEMF treatment during the 7 day postoperative period compared with the control treatment group (P = .010) with codeine administered 1.8 times more frequently in the control group. No untoward effects were recorded in either treatment group. More frequent evaluation of outcome measures with larger patient numbers, as well as histologic samples, may be useful in future studies. Dogs receiving PEMF therapy following postoperative hemilaminectomy demonstrated improved wound scores at 6 wk and reduced mean number of owner-administered pain medications compared with the control group therapy.
Phenotypic Effects of FGF4 Retrogenes on Intervertebral Disc Disease in Dogs. Kevin Batcher, Peter Dickinson, Michelle Giu rida, Beverly Sturges, Karen Vernau, Marguerite Knipe, Sheida Hadji Rasouliha, Cord Drögemüller, Tosso Leeb, Kimberly Maciejczyk, Christopher A. Jenkins, Cathryn Mellersh, Danika Bannasch. Genes. June 2019; doi: 10.3390/genes10060435. Quote: Two FGF4 retrogenes on chromosomes 12 (12-FGF4RG) and 18 (18-FGF4RG) contribute to short-limbed phenotypes in dogs. 12-FGF4RG has also been associated with intervertebral disc disease (IVDD). Both of these retrogenes were found to be widespread among dog breeds with allele frequencies ranging from 0.02 to 1; however, their additive contribution to disease is unknown. Surgical cases of IVDD (n = 569) were evaluated for age of onset, disc calcification, and genotypes for the FGF4 retrogenes. Multivariable linear regression analysis identified the presence of one or two copies of 12-FGF4RG associated with significantly younger age at first surgery in a dominant manner. 18-FGF4RG had only a minor effect in dogs with one copy. Multivariable logistic regression showed that 12-FGF4RG had an additive effect on radiographic disc calcification, while 18-FGF4RG had no effect. Multivariable logistic regression using mixed breed cases and controls identified only 12-FGF4RG as highly associated with disc herniation in a dominant manner (Odds Ratio, OR, 18.42, 95% Confidence Interval (CI) 7.44 to 50.26; p < 0.001). The relative risk for disc surgery associated with 12-FGF4RG varied from 5.5 to 15.1 within segregating breeds and mixed breeds. The FGF4 retrogene on CFA12 acts in a dominant manner to decrease the age of onset and increase the overall risk of disc disease in dogs. Other modifiers of risk may be present within certain breeds, including the FGF4 retrogene on CFA18.
Clinical, diagnostic imaging, surgical findings and long-term
outcome in a Cavalier King Charles Spaniel with thoracolumbar vertebral
articular process hyperplasia. Fabio Stabile, Robert
Brash, Luisa De Risio. Vet. REc. Case Repts. October 2019;7(4):e000932.
Quote: A 2-year-old female spayed Cavalier King Charles Spaniel
presented with 10-day history of progressive painful T3–L3 myelopathy. MRI
of the spine revealed an extradural dorsal spinal cord compression at the
level of T12–T13 vertebrae caused by hyperplasia of the caudal vertebral
articular process (CVAP) of T12 vertebra. Similar changes were noticed at
the level of the T13–L1 vertebrae, not causing spinal cord compression. In
order to plan surgical decompression, CT of the spine was performed. This
revealed thickened T12 dorsal lamina, hyperplastic T12 CVAP, and narrowed
and elongated T13 VAP. The patient underwent T12–T13 dorsal laminectomy and
spinal cord decompression by removal of the hyperplastic CVAP of T12.
Postoperative 6-year follow-up revealed a normal neurological examination. A
combination of MRI and CT allowed optimal treatment selection and surgical
planning for CVAP hyperplasia. Surgical treatment by dorsal laminectomy
provided successful long-term
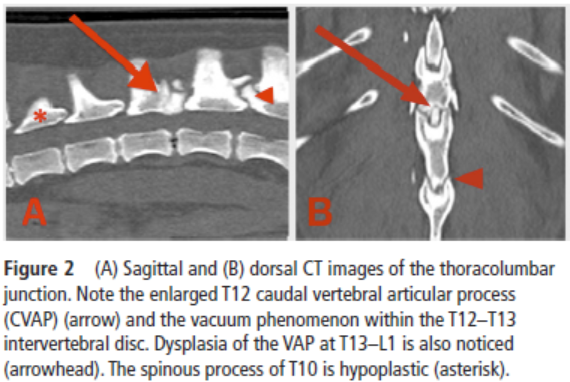 outcome.
... The day after surgery, the patient showed pelvic limb proprioceptive
ataxia and ambulatory paraparesis. On discharge 3 days after surgery, the
degree of ataxia and paresis were mildly improved compared with preoperative
examination. After 4 weeks of strict restriction in exercise and
postsurgical analgesia with meloxicam 0.1 mg/kg/24 h and gabapentin 10
mg/kg/8 h, the patient had a normal posture and a mild degree of
roprioceptive ataxia. Paw positioning and hopping were mildly delayed on the
pelvic limbs. At 2-month postoperative follow-up, the patient’s postural
reactions were normal and the gait was slightly ataxic in the pelvic limbs.
Follow-up at 1 year, 3 years and 6 years after surgery revealed normal
posture, normal gait and normal proprioception on both pelvic limbs. The
patient remained comfortable, exercising without restrictions. ... This is
the first report of a successful outcome after surgical treatment for focal
T3–L3 myelopathy caused by thoracic CVAP hyperplasia in a young CKCS
with a 6-year long-term follow-up. ... In our patient, a CKCS
of 10 kg of body weight, no changes compatible with DJD [degenerative joint
disease] were identified supporting the hypothesis that this patient was
more likely affected by a primary form of CVAP hyperplasia. The authors
consider that this is also supported by the fact that the similar changes
seen at T13–L1 did not cause any clinical signs over the long-term
follow-up.
outcome.
... The day after surgery, the patient showed pelvic limb proprioceptive
ataxia and ambulatory paraparesis. On discharge 3 days after surgery, the
degree of ataxia and paresis were mildly improved compared with preoperative
examination. After 4 weeks of strict restriction in exercise and
postsurgical analgesia with meloxicam 0.1 mg/kg/24 h and gabapentin 10
mg/kg/8 h, the patient had a normal posture and a mild degree of
roprioceptive ataxia. Paw positioning and hopping were mildly delayed on the
pelvic limbs. At 2-month postoperative follow-up, the patient’s postural
reactions were normal and the gait was slightly ataxic in the pelvic limbs.
Follow-up at 1 year, 3 years and 6 years after surgery revealed normal
posture, normal gait and normal proprioception on both pelvic limbs. The
patient remained comfortable, exercising without restrictions. ... This is
the first report of a successful outcome after surgical treatment for focal
T3–L3 myelopathy caused by thoracic CVAP hyperplasia in a young CKCS
with a 6-year long-term follow-up. ... In our patient, a CKCS
of 10 kg of body weight, no changes compatible with DJD [degenerative joint
disease] were identified supporting the hypothesis that this patient was
more likely affected by a primary form of CVAP hyperplasia. The authors
consider that this is also supported by the fact that the similar changes
seen at T13–L1 did not cause any clinical signs over the long-term
follow-up.
Intervertebral disc disease and aortic thromboembolism are the most common causes of acute paralysis in dogs and cats presenting to an emergency clinic. Graham Rossi, Alexandra Stachel, Alex M Lynch, Natasha J Olby. Vet. REc. May 2020; doi: 10.1136/vr.105844. Quote: Background: Acute paralysis is a common presentation in small animal emergency clinics, but the aetiological prevalence has not been reported. Knowledge of diagnosis frequency aids prioritisation of differential diagnoses, facilitates resource planning and clinical trial design. Methods: Medical records from NC State Veterinary Hospital Emergency Room were searched over a five-year period to identify cases presenting with acute non-ambulatory paraparesis or paralysis. Signalment and diagnosis category were extracted. Results: Acute paralysis was the presenting problem in 845 of 21,535 (3.9 per cent) dogs and 66 of 4589 (1.4 per cent) cats admitted over this period. Intervertebral disc disease (IVDD) was the most common cause (608 of 845; 72 per cent) in dogs, followed by vascular disease (34 of 845; 4.0 per cent). Other diagnostic categories accounted for the remaining 20 per cent. Dachshunds were the most common breed (263 of 845; 31.1 per cent), then Labrador retrievers (57 of 845; 6.7 per cent). In cats, aortic thromboembolism (ATE) was the most common diagnosis, occurring in 40 of 66 (60.6 per cent), followed by IVDD (7 of 66; 10.6 per cent). Other diagnostic categories accounted for 30.3 per cent. Six of 845 (0.7 per cent) dogs and two of 66 (3 per cent) cats were categorised as pseudoparalysis with a non-neurological diagnosis. Conclusions: IVDD and ATE are the overwhelming causes of acute paralysis in dogs and cats, respectively, with approximately 28 per cent of dogs and 40 per cent of cats having a different diagnosis.
Retrospective Study of 240 Dogs Receiving Gabapentin for Chronic Pain Relief. Lily V Davis, Peter W Hellyer, Robin A Downing, Lori R Kogan. J. Vet.Med. & Research. August 2020;7(4):1194-1197. Quote: Our goal was to assess gabapentin dosage and tolerability in dogs taking it for chronic pain. ... All patients in this study were on gabapentin due to an inability to fully control their pain with NSAIDs or nutraceuticals alone. ... The majority (217 patients; 90.42%) had pain localized to their back. The other anatomic locations of pain included stifle (33; 13.8%), elbow/shoulder (21; 8.8%) and hip (11; 4.6%). Some patients’ pain was localized to multiple areas and is counted in all categories. The most common diagnosis of pain was osteoarthritis (203; 84.6%), followed by generalized, nonspecific back pain (22;9.2%), intervertebral disk disease (18; 7.5%), and degenerative myelopathy (11; 4.6%). Some patients experienced two different kinds of pain and are embodied in both categories. One hundred and thirty-six (56.67%) patients did not have definitive anatomic cause for their pain, such as cruciate tears or intervertebral disc disease, as seen in Table 2. ... We retrospectively analyzed the medical records of 240 dogs taking gabapentin for chronic pain and systematically assessed: patient signalment, definitive diagnosis, location and description of pain, VAS scores immediately preceding and following the patient’s maximum gabapentin dose, maximum gabapentin dosage, presence or absence of side effects related to gabapentin use, use of NSAID/immunomodulator drugs and nutraceuticals, presence or absence of levothyroxine supplementation, surgical procedures, and physical medicine. The range of tolerated gabapentin doses was 6.9 - 500 mg/kg/day [3.1- 227.3 mg/lb], PO, q12 hr (every 12 hrs) and only 10% of patients experienced the most common side effect of sedation. ... The results from this case series suggest that gabapentin is well-tolerated at much higher doses than what is typically prescribed. Side effects were uncommon, with no clear pattern based on dose, or dog size or age. Therefore, like many other analgesic medications, the efficacy of gabapentin appears patient-specific and should be dosed to effect until side effects are noted or analgesia is achieved.
Classification of Intervertebral Disc Disease. Joe Fenn, Natasha J. Olby, the Canine Spinal Cord Injury Consortium. Front. Vet. Sci. October 2020; doi: 10.3389/fvets.2020.579025. Quote: Intervertebral disc disease (IVDD) is a broad term that is widely used in veterinary medicine and encompasses a range of lesions affecting the intervertebral disc. ... Whilst there are still many controversies in the categorization of types of disc-associated lesions in veterinary medicine, in this article we aim to review the relevant literature and to outline a consensus where possible. We will provide an up to date overview of reported types of IVDD, highlighting important features, and aiming to explain the theories behind their classification.
Diagnostic Imaging in Intervertebral Disc Disease. Ronaldo C. da Costa, Steven De Decker, Melissa J. Lewis, Holger Volk, the Canine Spinal Cord Injury Consortium (CANSORT-SCI). Front. Vet. Sci. October 2020; 7:588338. Quote: Imaging is integral in the diagnosis of canine intervertebral disc disease (IVDD) and in differentiating subtypes of intervertebral disc herniation (IVDH). These include intervertebral disc extrusion (IVDE), intervertebral disc protrusion (IVDP) and more recently recognized forms such as acute non-compressive nucleus pulposus extrusion (ANNPE), hydrated nucleus pulposus extrusion (HNPE), and intradural/intramedullary intervertebral disc extrusion (IIVDE). Many imaging techniques have been described in dogs with roles for survey radiographs, myelography, computed tomography (CT), and magnetic resonance imaging (MRI). Given how common IVDH is in dogs, a thorough understanding of the indications and limitations for each imaging modality to aid in diagnosis, treatment planning and prognosis is essential to successful case management. While radiographs can provide useful information, especially for identifying intervertebral disc degeneration or calcification, there are notable limitations. Myelography addresses some of the constraints of survey radiographs but has largely been supplanted by cross-sectional imaging. Computed tomography with or without myelography and MRI is currently utilized most widely and have become the focus of most contemporary studies on this subject. Novel advanced imaging applications are being explored in dogs but are not yet routinely performed in clinical patients. The following review will provide a comprehensive overview on common imaging modalities reported to aid in the diagnosis of IVDH including IVDE, IVDP, ANNPE, HNPE, and IIVDE. The review focuses primarily on canine IVDH due to its frequency and vast literature as opposed to feline IVDH.
Lumbosacral intervertebral disk extrusions in 13 dogs. Luca Bresciani, Raquel Trevai,, Stephen Clarke, Rodrigo Gutierrez-Quintana, Sebastien Behr, Kali Lazzerini, Josep Brocal, Bill Oxley, Jonathan Pink, Roberto José-López. Vet. Surgery. March 2021; doi: 10.1111/vsu.13624. Quote: Objective: To describe the clinical presentation, magnetic resonance imaging (MRI) findings, and outcome of dogs treated surgically for lumbosacral intervertebral disk extrusion (IVDE). Study Design: Retrospective study. Animals: Thirteen dogs [including one cavalier King Charles spaniel]. Methods: Records and MRI studies of dogs with intraoperatively confirmed lumbosacral IVDE were reviewed. MRI features of thoracolumbar IVDE were applied to all cases. Postoperative outcome was subjectively assessed as excellent, good, or poor. Results: All dogs had an acute or subacute onset of lumbosacral pain and nerve root signature. Seven dogs had neurological deficits [including the CKCS]. MRI revealed lateralized herniated disk material and partial to complete disk degeneration in all cases; the extradural material extended cranial and/or caudally from the disk space in 10 cases. All dogs underwent L7-S1 dorsal laminectomy and removal of extruded disk material. In six dogs, surgery was complicated by inflammatory changes [including the CKCS], including one case of epidural steatitis. On reexamination 4–6 weeks postsurgery, outcome was judged as excellent in 11 dogs [including the CKCS] and poor in the remaining 2 due to contralateral nerve root signature in one case and nonambulatory paraparesis and urinary incontinence in the case with steatitis. Conclusion: Lumbosacral IVDE in dogs was characterized by acute/subacute onset of lumbosacral pain and nerve root signature and lateralized and often dispersed extradural material over a degenerated L7-S1 intervertebral disk on MRI. Early decompressive dorsal laminectomy generally resulted in excellent clinical outcome. Clinical Significance: Observation of these clinical and imaging features in dogs should prompt clinical suspicion of lumbosacral IVDE.
The Effects of FGF4 Retrogenes on Canine Morphology. Danika Bannasch, Kevin Batcher, Fabienne Leuthard, Michael Bannasch, Petra Hug, Denis J. Marcellin-Little, Peter J. Dickinson, Michaela Drögemüller, Cord Drögemüller, Tosso Leeb. Genes. February 2022; doi: 10.3390/genes13020325. Quote: Two FGF4 retrogenes (FGF4L1 on chromosome 18 and FGF4L2 on chromosome 12) have been identified to cause dwarfism across many dog breeds. Some breeds are nearly homozygous for both retrogenes (e.g., Dachshunds) and others are homozygous for just one (e.g., Beagles and Scottish Terriers). Since most breeds do not segregate both of these retrogenes, it is challenging to evaluate their individual effects on long bone length and body size. We identified two dog breeds selected for hunting ability, the Alpine Dachsbracke and the Schweizer Niederlaufhund, that segregate both of these retrogenes. Using individual measurements of height at the shoulder, back length, head width, thorax depth and width, and thoracic limb measurements, we evaluated the combined effects of FGF4 retrogenes within these breeds. We applied multivariable linear regression analysis to determine the effects of retrogene copy numbers on the measurements. Copy numbers of both retrogenes had significant effects reducing height at the shoulders and antebrachial length, with FGF4L1 having a much greater effect than FGF4L2. FGF4L1 alone influenced the degree of carpal valgus and FGF4L2 alone increased head width. Neither retrogene had an effect on thorax width or depth. Selectively breeding dogs with FGF4L1 and without FGF4L2 would likely lead to a reduction in the FGF4L2-related risk of intervertebral disc herniation while maintaining the reduction in leg length resulting from FGF4L1.
Postoperative outcome of ambulatory dogs with intervertebral disc extrusion causing incontinence and/or tail dysfunction: 18 cases (2010-2020). R. Pfund, A. K. Forward, R. Fentem, A. Nagendran, A. R. Fraser, A. H. Crawford. J. Sm. Anim. Pract. July 2022; doi: 10.1111/jsap.13497. Quote: Objectives: To assess the recovery of urinary continence, faecal continence and tail function in ambulatory dogs with caudal lumbar intervertebral disc extrusion and to explore clinical factors that may be associated with recovery. Materials and Methods: Medical records from January 2010 to December 2020 were searched to identify ambulatory dogs undergoing surgical treatment for a caudal lumbar intervertebral disc extrusion causing urinary incontinence, faecal incontinence and/or tail dysfunction. Signalment, history, presenting clinical signs, neurological examination findings, diagnostic test results, treatment and outcome were recorded for all dogs. Results: Eighteen dogs with caudal lumbar intervertebral disc extrusion causing tail dysfunction, urinary and/or faecal incontinence were included. ... Affected breeds were four (22%) Cavalier King Charles Spaniels, four (22%) cocker spaniels, three (17%) dachshunds, two (11%) crossbreeds, one (6%) French bulldog, Belgian Laekenois, Pug, German shepherd dog and Pomeranian. ... Cocker spaniels and Cavalier King Charles spaniels appeared to be over-represented, accounting for eight of 18 (44%) dogs in this case series. ... Urinary continence was recovered in 12 (86%) of 14 affected dogs [including 2 of the CKCS], faecal continence recovered in nine (90%) of 10 affected dogs [including 2 of the CKCS] and tail function recovered in 13 (87%) of 15 affected dogs [including 1 CKCS]. Loss of tail nociception was recorded in three dogs on presentation; two made a full recovery and one showed mild persistent tail paresis. Clinical Significance: The prognosis for functional recovery of urinary continence, faecal continence and tail function in ambulatory dogs with caudal lumbar intervertebral disc extrusion following surgical treatment is good. Larger studies are needed to identify prognostic factors associated with failure of recovery.
ACVIM consensus statement on diagnosis and management of acute canine thoracolumbar intervertebral disc extrusion. Sarah A. Moore, Natasha J. Olby, Brigitte Brisson, Joe Fenn, Thomas Flegel, Gregg Kortz, Melissa Lewis, Andrea Tipold. J. Vet. Intern. Med. July 2022; doi: 10.1111/jvim.16480. Quote: Background: Thoracolumbar intervertebral disc extrusion (TL-IVDE) is the most common cause of acute paraparesis and paraplegia in dogs; however, guidelines on management of the condition are lacking. Objectives: To summarize the current literature as it relates to diagnosis and management of acute TL-IVDE in dogs, and to formulate clinically relevant evidence-based recommendations. Methods: A panel of 8 experts was convened to assess and summarize evidence from the peer-reviewed literature in order to develop consensus clinical recommendations. Level of evidence available to support each recommendation was assessed and reported. Results: The majority of available literature described observational studies. Most recommendations made by the panel were supported by a low or moderate level of evidence, and several areas of high need for further study were identified. These include better understanding of the ideal timing for surgical decompression, expected surgical vs medical outcomes for more mildly affected dogs, impact of durotomy on locomotor outcome and development of progressive myelomalacia, and refining of postoperative care, and genetic and preventative care studies. Conclusions and Clinical Importance: Future efforts should build on current recommendations by conducting prospective studies and randomized controlled trials, where possible, to address identified gaps in knowledge and to develop cost effectiveness and number needed to treat studies supporting various aspects of diagnosis and treatment of TL-IVDE.

Spontaneous vocalization in dogs presenting for neurological evaluation between 2016 and 2022: A descriptive study. A. Spencer-Taylor, P. Freeman, L. Alves, A. Vanhaesebrouck, S. Khan, G. Harris. 34th Symposium ESVN-SCVN; QB10. J. Vet. Intern. Med. September 2022; doi: 10.1111/jvim.17218. Quote: Introduction Spontaneous vocalization has been anecdotally associated with cervical disc disease and more robustly associated with Chiari-like malformation and syringomyelia. This study describes the signalment, localisation and diagnoses in a cohort of dogs presenting with spontaneous vocalization. Methods The records of dogs presenting to the neurology department between 2016 and 2022 with spontaneous vocalization as a presenting sign were reviewed and analyzed. Spontaneous vocalization was defined as a sudden, highpitched sound when moving or at rest without an obvious inciting cause. Dogs were excluded if vocalization was an isolated episode, initiated by palpation or was associated with strenuous activity. Results 59 dogs met the inclusion criteria, 44 were male, 40 were neutered and the median age at presentation was 63 months (4–348). French Bulldog (n = 10), crossbreed (n = 8), and Cavalier King Charles Spaniel (n = 7) were the three commonest breeds. The most prevalent localisation was C1–C5 (n = 17). The most frequent diagnoses were intervertebral disc herniation (n = 26), syringomyelia (n = 6), neoplasia (n = 5), and atlantoaxial instability (n = 4). Of the 33 dogs localized to the cervical spine, intervertebral disc herniation was found in 18 of them. DiscussionIn this cohort of dogs, spontaneous vocalization was most frequently associated with a localisation of the cervical spine (more specifically C1-C5) and a diagnosis of intervertebral disc herniation. Of those dogs that localized to the cervical spine an intervertebral disc herniation was the most likely diagnosis (18/33). Incorporating this information into a clinical reasoning framework may aid in clinical decision making especially when advanced imaging is unavailable.
Retrospective study of acupuncture treatment for canine thoracolumbar intervertebral disc herniation. Qianyu Jia, Yu Wang, Haidong Pang, Kai Fan, Huisheng Xie, Jiahao Lin. One Health Advances. September 2023; doi: 10.1186/s44280-023-00022-y. Quote: Thoracolumbar interverbal disk herniation (TL-IVDH) is a common neurological disorder in dogs, which often affects the life quality of patients and their caregivers. Acupuncture is increasingly accepted by veterinarians and animal owners, and has been used in the treatment of neurologic disorders. This study aims to evaluate the effects of acupuncture treatment for canine TL-IVDH. Clinical cases from 2016 to 2021 were collected. According to the inclusion and exclusion criteria, 94 TL-IVDH cases that received acupuncture treatment were selected. Clinical classification and efficacy criteria were formulated based on the Frankel Score. For each case, clinical presentation, improvement, recovery and recurrence were recorded. Male dogs with TL-IVDH accounted for 64% of all cases. The average age was 7.49 years old, the predominant breed was poodle, and the incidence site was concentrated from T11 to L1. The overall recovery rate after receiving acupuncture treatment was 79.78%, which was comparable when considering only cases with grade 2, 3, or 4 spinal cord lesions (83.33% ~ 85.19%). In conclusion, canine with grade 2, 3, and 4 spinal cord lesions due to TL-IVDH receiving acupuncture had a high recovery rate, suggesting acupuncture could be a viable treatment options for canine with TL-IVDH. ... In conclusion, the total recovery rate of acupuncture treatments in this study was 79.78%, which is significantly higher than that of conservative treatment recovery rates reported in previous studies. Deep pain perception is the most important factor for the efficacy of acupuncture on IVDH functional recovery. Additionally, the age of patients, those with recurrent disease, and the frequency of acupuncture treatments also affected the recovery outcome.
Clinical and imaging findings in dogs with nerve root signature associated with cervical intervertebral disc herniation. Jordan Schachar, Alan Bocage, Nathan C. Nelson, Peter J. Early, Christopher L. Mariani, Natasha J. Olby, Karen R. Muñana. J. Vet. Intern. Med. January 2024; doi: 10.1111/jvim.16982. Quote: Background: Intervertebral disc herniation (IVDH) is the most common spinal cord disease in dogs. Little information is available regarding the clinical presentation of nerve root signature (NRS) associated with cervical IVDH. Hypothesis/Objective: To detail the clinical and magnetic resonance imaging (MRI) findings in dogs with NRS associated with cervical IVDH. Animals: Forty-seven client-owned dogs presenting with thoracic limb NRS and MRI confirmed IVDH [incluidng one cavalier King Charles spaniel]. Methods: Medical records from 2010 to 2020 were retrospectively reviewed for dogs that met inclusion criteria. Imaging studies were evaluated by 2 individuals to characterize location and severity of neural tissue compression. Results: Chondrodystrophoid dogs comprised the majority of the study cohort, with dachshund the most common breed (n=10). Three-quarters of dogs were ≥7 years of age. Interobserver agreement was moderate or good for all of the imaging variables evaluated. The C6-C7 intervertebral disc space was significantly overrepresented, comprising 32% (15/47) of the affected discs. However, 42% (20/47) of cases involved C2-C3 though C4-C5 disc sites. Disc material was more frequently located laterally compared to medially within the vertebral canal, and to be associated with compression of the nerve root at the level of the intervertebral foramen. Conclusion/Clinical Importance: NRS is most commonly associated with lateralized or foraminal cervical disc herniations. It is most prevalent with C6-C7 intervertebral disc involvement, suggesting that there might be unique anatomic factors that contribute to development of NRS at this site, but can be a clinical manifestation of IVDH occurring anywhere along the cervical spine.
Spontaneous resorption of a C7–T1 intervertebral disc extrusion in a
Cavalier King Charles spaniel confirmed via low-field MRI.
Michelle du Toit, Neringa Alisauskaite. Vet. Rec. February 2024; doi:
10.1002/vrc2.812. Quote: A 4-year-old,
 male,
neutered Cavalier King Charles spaniel was referred to the
neurology service with a 10-day history of cervical hyperaesthesia. A
low-field magnetic resonance imaging scan of the cervical spine identified a
large C7–T1 intervertebral disc extrusion, resulting in severe spinal cord
compression.The patient was treated with conservative therapy (exercise
restriction and analgesia for 4 weeks). Repeat magnetic resonance imaging of
the cervical spine was performed 4 months after initial presentation, and
identified spontaneous resorption of the extruded C7–T1 disc material. There
are very few documented cases of spontaneously resorbed cervical
intervertebral disc extrusions in canine patients following successful
conservative therapy. To the authors’ knowledge, this is the first report of
spontaneous resorption of an intervertebral disc extrusion at an unusual
C7–T1 location confirmed via follow-up low-field magnetic resonance imaging
following conservative therapy.
male,
neutered Cavalier King Charles spaniel was referred to the
neurology service with a 10-day history of cervical hyperaesthesia. A
low-field magnetic resonance imaging scan of the cervical spine identified a
large C7–T1 intervertebral disc extrusion, resulting in severe spinal cord
compression.The patient was treated with conservative therapy (exercise
restriction and analgesia for 4 weeks). Repeat magnetic resonance imaging of
the cervical spine was performed 4 months after initial presentation, and
identified spontaneous resorption of the extruded C7–T1 disc material. There
are very few documented cases of spontaneously resorbed cervical
intervertebral disc extrusions in canine patients following successful
conservative therapy. To the authors’ knowledge, this is the first report of
spontaneous resorption of an intervertebral disc extrusion at an unusual
C7–T1 location confirmed via follow-up low-field magnetic resonance imaging
following conservative therapy.
Demographic and lifestyle characteristics impact lifetime prevalence of owner-reported intervertebral disc disease: 43,517 companion dogs in the United States. Crystal Wee, Darren Z. Nin. J. Amer. Vet. Med. Assn. January 2025; doi: 10.2460/javma.24.08.0553. Quote: Objective: Intervertebral disc disease (IVDD) is a debilitating spinal condition that has been well studied among Dachshunds. However, little is known about IVDD prevalence across other dog breeds and associated lifestyle risk factors. The purpose of this study was to identify lifetime prevalence, demographic, and lifestyle factors associated with IVDD among a large population of companion dogs in the US. Methods: An observational cross-sectional study was conducted with the Dog Aging Project database. Companion dogs enrolled between December 26, 2019, and December 31, 2022, were included. The primary outcome was lifetime prevalence of owner-reported IVDD (OR-IVDD). Associations between OR-IVDD, demographic, and lifestyle factors were evaluated with multivariate logistic regression. Results: 43,517 dogs (female, 49.6% [21,582 of 43,517]; purebred, 50.3% [21,910 of 43,517]) were included in the study. Lifetime prevalence of OR-IVDD was 1.2% (520 of 43,517). On adjusted analysis, male (OR, 1.36; 95% CI, 1.13 to 1.64), purebred (OR, 1.66; 95% CI, 1.37 to 2.01), toy and small (OR, 1.85; 95% CI, 1.51 to 2.27), and overweight (OR, 1.67; 95% CI, 1.38 to 2.01) dogs had increased odds of OR-IVDD. Lifestyle factors associated with reduced odds of OR-IVDD include higher daily active time, being on a commercial diet, and regular use of a staircase. Dachshunds had the highest lifetime prevalence of OR-IVDD (15.3% [83 of 541]). Among purebred dogs, French Bulldogs had the highest odds of OR-IVDD (OR, 21.1; 95% CI, 12.5 to 35.8) on adjusted analysis. After adjustment for age, sex, and sterilization status, French Bulldogs, Dachshunds, Beagles, Cavalier King Charles Spaniels, and Newfoundlands had increased odds of OR-IVDD compared to mixed-breed dogs. Conclusions: Owner-reported IVDD is impacted by demographic and lifestyle factors such as breed status, daily active time, and staircase use. Clinical Relevance: An increased focus on breed-specific research of French Bulldogs would be beneficial considering breed popularity and lifetime prevalence of OR-IVDD. Further longitudinal research is needed to assist with clinical decision-making and lifestyle recommendations.
Percutaneous enzymatic chemonucleolysis of intervertebral disks appears safe and effective in treatment of acute-onset paraparesis and paraplegia in small dogs. Paul Freeman, Genna Atiee, Eileen M. Donoghue, Nick D. Jeffery. J. Amer. Vet. Med. Assn. March 2025; doi:10.2460/javma.24.12.0790. Quote: Objective: To investigate the safety and effectiveness of intradiscal chondroitinase injection as a pragmatic treatment for nonambulatory paraparesis and paraplegia in small dogs. Methods: In this phase 1 clinical trial, dogs presented to 2 university neurology clinics between January 2023 and June 2024 with acute-onset nonambulatory paraparesis or paraplegia occurring within 48 hours before presentation. Included animals weighed < 15 kg and were between 2 and 10 years old, with caregivers who were unable to afford decompressive surgery. Under fluoroscopic guidance, each dog received 1.25 U of chondroitinase ABC into each of 4 consecutive intervertebral disks in the clinically identified lesion location. Recovery was defined as the ability to walk 50 steps without assistance by 4 months after the injection. Results: 54 dogs were included, with 4 lost to sufficient follow-up. In those with appropriate follow-up, 38 of 40 dogs (proportion, 0.95; 95% CI, 0.83 to 1.00) with intact pain sensation to the hindquarters recovered by a median of 11 days after the intervention, and 4 of 10 dogs (0.4; 95% CI, 0.17 to 0.69) without pain sensation recovered. No adverse effects related to the injection procedure were detected. Conclusions: In dogs with intact pain perception, this nonsurgical intervention is associated with similar proportion and time to recover as decompressive surgery. Because of the small case number, uncertainty remains regarding the effectiveness of this intervention in dogs in which hindquarter pain perception has been lost. Clinical Relevance: Nonsurgical treatment for presumed disc-associated paresis and paraplegia appears promising. Randomized controlled trials are required for assessment of effectiveness versus decompressive surgery.
Association of the FGF4L2 retrogene with fibrocartilaginous embolic myelopathy in dogs. Colleen Embersics, Danika Bannasch, Kevin Batcher, Elizabeth C. Boudreau, Molly Church, Andrew Miller, Simon Platt, Jey Koehler, Natasha Olby, John Rossmeisl, Daniel Rissi, Robert Grahn, Jonas Donner, Peter J. Dickinson. J. Vet. Intern. Med. November 2023; doi: 10.1111/jvim.16925. Quote: Background: Fibrocartilaginous embolic myelopathy (FCE) is a well-documented condition in dogs although rarely reported in chondrodystrophic breeds. Genetic associations have not been defined. Objectives: Define the association of the chondrodystrophy-associated FGF4L2 retrogene with histopathologically confirmed cases of FCE. Animals: Ninety-eight dogs with a histopathologic diagnosis of FCE. Methods: Retrospective multicenter study. Dogs were genotyped for the FGF4L2 and FGF4L1 retrogenes using DNA extracted from formalin-fixed, paraffin-embedded tissue. Associations between breed, FCE and retrogene status were investigated with reference to a hospital population and known breed and general population allele frequencies. Results: FGF4L2 genotype was defined in 89 FCE cases. Fibrocartilaginous embolic myelopathy was present in 22 dogs from FGF4L2-segregating breeds with allele frequencies of ≥5%; however, all dogs were wild type. Two Labrador retrievers with FCE carried FGF4L2 alleles. Frequency of the FGF4L2 allele was significantly (P < .001) and negatively associated with FCE relative to predicted hospital-population dogs. FCE was overrepresented in Boxer, Great Dane, Yorkshire Terrier, Bernese Mountain Dog, Miniature Schnauzer, Rottweiler, and Shetland Sheepdog breeds. Conclusions and Clinical Importance: Study data based on genotypically and histopathologically defined cases support the historical observation that FCE is uncommon in chondrodystrophic dog breeds. FGF4 plays an important role in angiogenesis and vascular integrity; anatomical studies comparing chondrodystrophic and non-chondrodystrophic dogs might provide insight into the pathogenesis of FCE.


CONNECT WITH US